Translate this page into:
Videodermoscopy: A useful diagnostic tool for cutaneous metastases of prostate cancer
Correspondence Address:
Marta Sar-Pomian
Department of Dermatology, Medical University of Warsaw, Koszykowa 82a, 02-008 Warsaw
Poland
| How to cite this article: Golinska JM, Sar-Pomian M, Rudnicka L. Videodermoscopy: A useful diagnostic tool for cutaneous metastases of prostate cancer. Indian J Dermatol Venereol Leprol 2020;86:565-568 |
Sir,
Prostate cancer is the second most common cancer in men.[1] Cutaneous metastases are observed in 0.1%–0.4% of patients with prostate adenocarcinoma.[1] No data are available regarding the dermoscopic evaluation of cutaneous metastases of this cancer in the literature.
A 78-year-old man presented to the Department of Dermatology of Medical University of Warsaw with unilateral violaceous patches, and erythematous nodules and plaques localized in the right thigh, inguinal area, lower abdomen and ipsilateral aspect of scrotum [Figure - 1]a and [Figure - 1]b. Skin lesions appeared one month prior to hospitalization and were associated with mild itching and a sensation of spreading over skin.
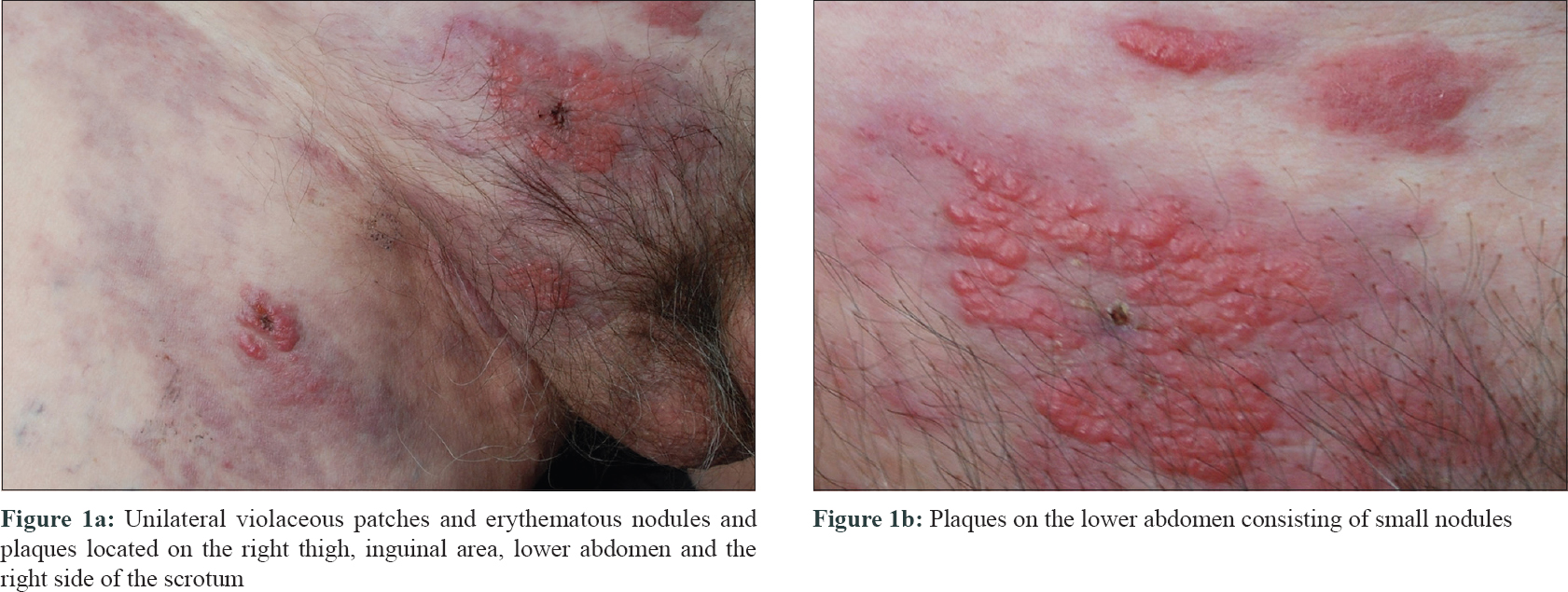 |
The patient was diagnosed with prostate adenocarcinoma in 2001 (Gleason's score 7 [3 + 4]).
Videodermoscopy (Fotofinder Medicam 1000, Bad Birnbach, Germany) of nodular lesions demonstrated white lines forming a network pattern on an orange-red background [Figure - 2]a. The use of 20-fold working magnification revealed the presence of dotted vessels surrounded by a whitish halo arranged linearly [Figure - 2]b. Coiled or comma-shaped appearance of dotted vessels was detected by videodermoscopy using 70-fold magnification [Figure - 2]c. Linear curved vessels and branching vessels were observed at the periphery of these nodules [Figure - 2]d.
 |
Dermoscopy of violaceous patches showed regularly distributed dotted vessels under 10-fold working magnification, while their linear curved shapes on the pinkish background could be delineated using 70-fold working magnification [Figure - 2]e.
Histopathology of both lesions (right thigh and lower right abdomen) revealed the presence of poorly differentiated cells forming tube-like structures with neurovascular invasion [Figure - 3].
 |
| Figure 3: Histopathological examination: poorly differentiated cells (asterisks) forming tubular-like structures (arrows) with a vascular invasion (triangles) (H and E, ×200) |
Cutaneous metastases of internal malignancies usually present as papules, nodules, plaques or ulcers near the anatomical region of the primary cancer. Our database search revealed one case report of onychoscopy of subungual metastasis of prostate cancer describing nonmelanocytic black pigmentation of the nail bed, with hematomas and vascular-like nodules, along with dilated blood vessels.[2]
The presence of vessels in cutaneous metastases results from tumor angiogenesis. Several vascular patterns have been observed by dermoscopy of skin metastases of varied origin.
Chernoff et al. described the presence of vessels in 15 (88%) nonpigmented and 1 (33%) pigmented skin metastasis in the analysis of 20 patients, who had a varied primary source including breast, colorectal, thyroid, ovarian, endometrial, gastric, lung, bladder and peritoneal cancers and leiomyosarcoma.[3] The most common presentation was linear curved vessels in 13 (77%) lesions, followed by arborizing vessels in nine (53%), dotted vessels in four (24%) and comma-shaped vessels in three (18%) cases.[3]
Ten (59%) pigmented skin metastases reported by Chernoff et al. presented more than one vascular pattern.[3] A combination of dotted and linear straight or linear curved vessels was reported most commonly.[3] The prominent dermoscopic features of nodules in our patient included the coexistence of central dotted vessels and peripheral linear-curved and branching vessels. Manganoni et al. reported the coexistence of multiple types of vessels in colon adenocarcinoma metastases with irregular linear and antler-like vessels in the center and dotted, hairpin and looped vessels at the periphery.[4]
Various patterns of vascular distribution have been reported in skin metastases by dermoscopy, irregular arrangement of vessels being the commonest.[3],[4] In our patient, dotted vessels were arranged linearly in the center of nodule, whereas irregular arrangement was noted at the periphery.
Apart from vascular abnormalities, we observed white lines in our patient. White lines are also reported in cutaneous metastases of renal cancer, suggestive of fibrosis.[5]
Our limitation was dermoscopic analysis of a single patient with cutaneous metastases of prostate cancer.
Dermoscopy may become a useful tool in the preliminary diagnosis of cutaneous metastases of prostate cancer. The diagnosis of skin metastases may be indicated by the presence of violaceous nodules on the abdomen, groin or upper thigh region with dermoscopy revealing a white network on an orange-red background, in combination with vascular abnormalities under video (dermoscopy), such as linearly or irregularly arranged dotted vessels surrounded by a whitish halo (showing coiled or comma-shaped appearance at higher magnification) in the center and linear curved and branching vessels at the periphery of lesion. We suggest incorporating dermoscopy in the examination of skin lesions in all patients with internal malignancies.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient has given his consent for his images and other clinical information to be reported in the journal. The patient understands that name and initials will not be published and due efforts will be made to conceal identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
| 1. |
Esquivel-PintoI A, Torres-Alvarez B, Gómez-Villa RJ, Castanedo-Cázares JP. A case of prostatic carcinoma manifesting as cutaneous facial nodule. Case Rep Urol 2018;2018:5265909.
[Google Scholar]
|
| 2. |
García-Galaviz R, Domínguez-Cherit J, Caro-Sánchez C, Salazar-Rojas E. Subungual metastasis of an adenocarcinoma of the prostate in a finger. Skin Appendage Disord 2018;5:46-9.
[Google Scholar]
|
| 3. |
Chernoff KA, Marghoob AA, Lacouture ME, Deng L, Busam KJ, Myskowski PL. Dermoscopic findings in cutaneous metastases. JAMA Dermatol 2014;150:429-33.
[Google Scholar]
|
| 4. |
Manganoni AM, Fusano M, Pavoni L, Pizzati L, Consoli F, Venturini M, et al. A solitary cutaneous metastasis from colon adenocarcinoma: Dermoscopic and confocal microscopy features. Indian J Dermatol Venereol Leprol 2018;84:589-91.
[Google Scholar]
|
| 5. |
Soares GH, Lallas A, Lombardi M, Longo C, Moscarella E, Raucci M, et al. Cutaneous metastasis of renal carcinoma. J Am Acad Dermatol 2015;72:S45-6.
[Google Scholar]
|
Fulltext Views
2,130
PDF downloads
562





