© Copyright 2024 – Indian Journal of Dermatology, Venereology and Leprology – All rights reserved.
Published by Scientific Scholar on behalf of Indian Association of Dermatologists, Venereologists & Leprologists (IADVL), India.
ISSN (Print): 0378-6323
ISSN (Online): 0973-3922














Commentary
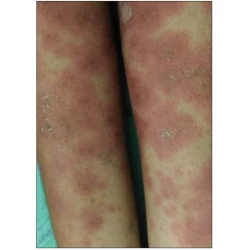
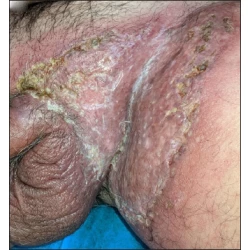
Scoring for palmoplantar psoriasis – need for modification of current methodology
Murlidhar Rajagopalan
DOI: 10.25259/IJDVL_485_2024
Full text |
|  PDF
PDF 