Translate this page into:
Primary follicular mucinosis in childhood
2 Department of Pathology, Kubba Skin Clinic, New Delhi, India
3 Department of Dermatology and STD, VMMC and Safdarjung Hospital, New Delhi, India
Correspondence Address:
Aditi Jha
Department of Dermatology Venereology and Leprosy, VMMC and Safdarjung Hospital, New Delhi
India
| How to cite this article: Verma P, Kubba A, Jha A. Primary follicular mucinosis in childhood. Indian J Dermatol Venereol Leprol 2019;85:333-334 |
A-10-year-old boy presented with hypopigmented soft plaque over the left lateral eyebrow and forehead for 5 months. There was complete loss of eyebrows in the involved area. Discrete brown follicular plugs were seen at the centre of the plaque [Figure - 1]. There was no history of atopy, sensory loss or systemic complaints. Biopsy from the centre of the plaque revealed follicular plugging, superficial and deep dense perifollicular infiltrate of lymphohistiocytes and mucin deposition within few hair follicles, favoring the diagnosis of follicular mucinosis. There were no atypical cells or epidermotropism. Staining for acid-fast bacilli was negative. He was started on medium-potency topical steroids. He remains under regular follow-up and after 3 months of initiating treatment there was partial improvement in pigmentation and no new lesions. The differentials that should be considered for follicular mucinosis are borderline tuberculoid hansens disease, especially in areas endemic for leprosy, lichen spinulosus, keratosis pilaris, lymphomas, lymphocytic infiltrates, etc., depending on the morphology of the lesion.
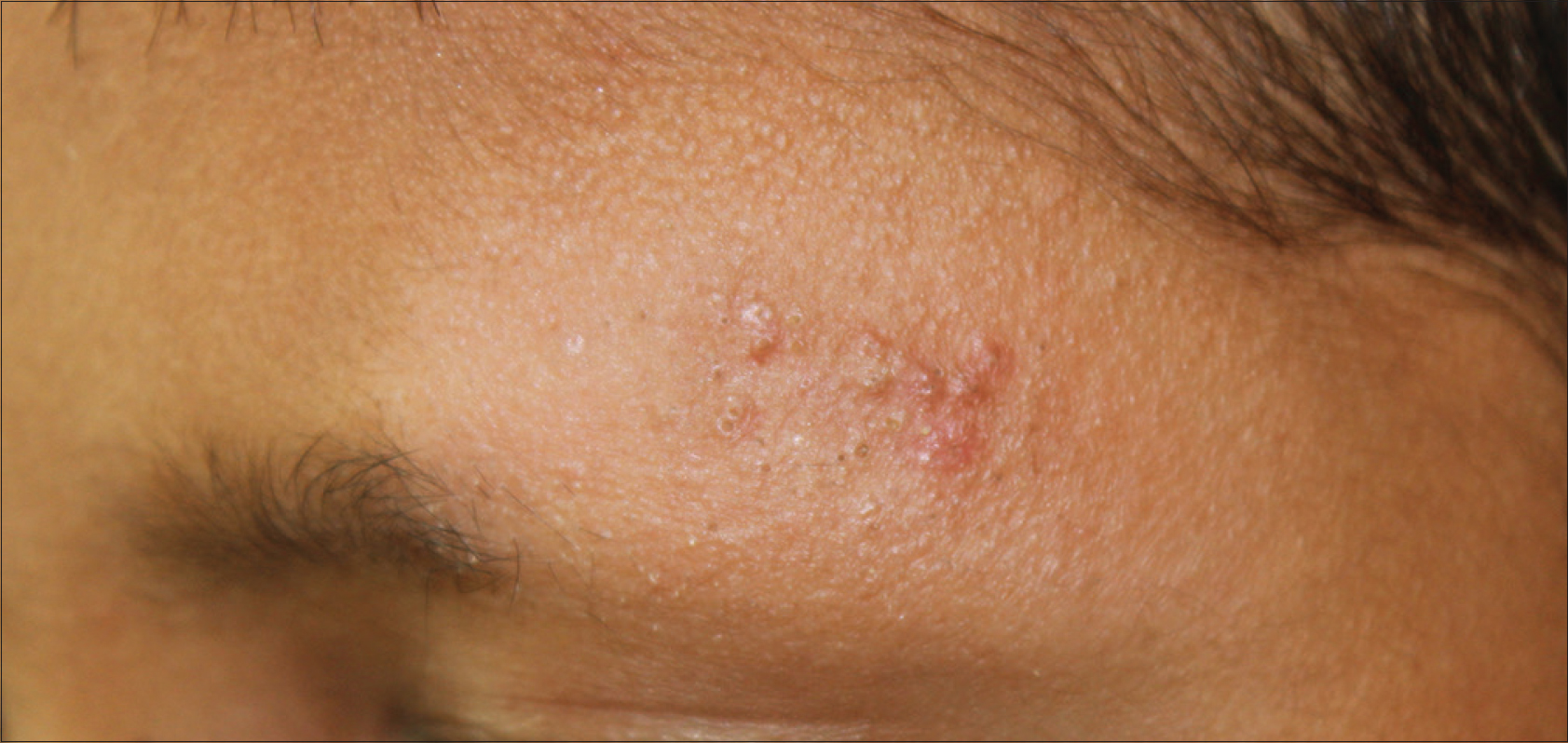 |
| Figure 1: (Clinical) Ill-defined hypopigmented plaque with loss of appendages and discrete brown follicular plugs seen in the centre |
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient has given his consent for his images and other clinical information to be reported in the journal. The patient understand that name and initials will not be published and due efforts will be made to conceal identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Fulltext Views
2,503
PDF downloads
1,064





