Translate this page into:
Bulla formation at the tuberculin skin test site in a patient with bullous pemphigoid: Koebnerization or severe delayed-type hypersensitivity?
2 Department of Histopathology, Postgraduate Institute of Medical Education and Research, Chandigarh, India
Correspondence Address:
Dipankar De
Department of Dermatology, Venereology and Leprology, Postgraduate Institute of Medical Education and Research, Sector 12, Chandigarh - 160 012
India
| How to cite this article: Bishnoi A, De D, Handa S, Mahajan R, Chatterjee D, Saikia UN. Bulla formation at the tuberculin skin test site in a patient with bullous pemphigoid: Koebnerization or severe delayed-type hypersensitivity?. Indian J Dermatol Venereol Leprol 2018;84:227-229 |
Sir,
Koebner's isomorphic phenomenon refers to the development of new lesions of a dermatosis (clinically and pathologically similar to the pre-existing dermatosis) at previously uninvolved sites after trauma. It has been classically described with psoriasis, vitiligo, and lichen planus, and is thought to represent active disease.[1] Reports of Koebner's phenomenon occurring in autoimmune bullous disorders are uncommon. Here, we report a case of bullous pemphigoid who developed Koebner's phenomenon at the site of tuberculin skin test.
A 60-year-old man presented with a 6-month-history of multiple scattered, tense, bullous lesions over an urticarial base. Histopathology and direct immunofluorescence on skin biopsy was suggestive of bullous pemphigoid. As a part of routine investigations being performed to initiate steroid sparing immunosuppressive treatment, it was observed that the site of tuberculin skin test on ventral aspect of upper left forearm developed a bullous reaction after 72 hours of injection of 5 units (0.1 ml) of purified protein derivative. The bulla was oval in shape, approximately 2 cm in diameter, tense, itchy, and contained serous fluid [Figure - 1]a and [Figure - 1]b. In view of normal contrast-enhanced computed tomographic scans of chest and abdomen, normal urine examination, and a negative history for tuberculosis, possibility of severe hypersensitivity to purified protein derivative was considered less likely. Two biopsies were taken, one from the margin of the bulla and another from perilesional skin, for histopathology and direct immunofluorescence examination, respectively. Histopathology showed a subepidermal split with eosinophils and neutrophils in blister cavity [Figure - 2]a. Direct immunofluorescence revealed a linear deposition of immunoglobulin G [Figure - 2]b and complement C3 [Figure - 2]c at basement membrane, consistent with bullous pemphigoid. There were no chronic inflammatory cell infiltrate, epitheloid cells or giant cells to suggest a positive hypersensitivity reaction to purified protein derivative.
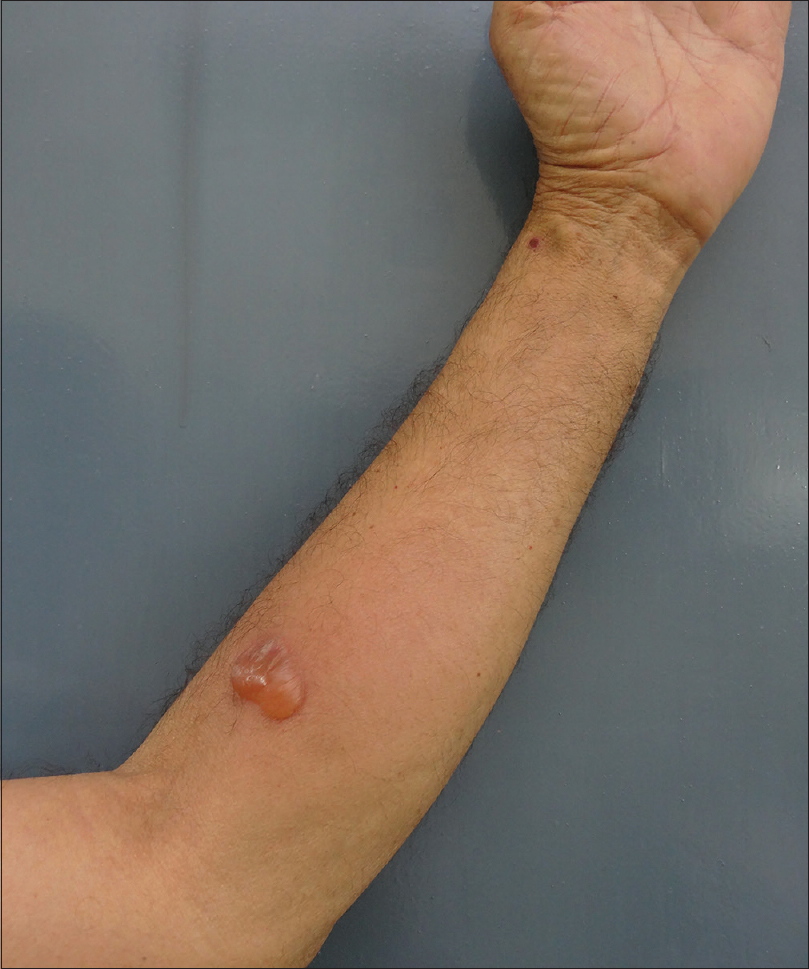 |
| Figure 1a: At the site of tuberculin skin testing, a tense bulla filled with serous fluid, around 2 cm × 2 cm size, developed 72 h after testing with purified protein derivative |
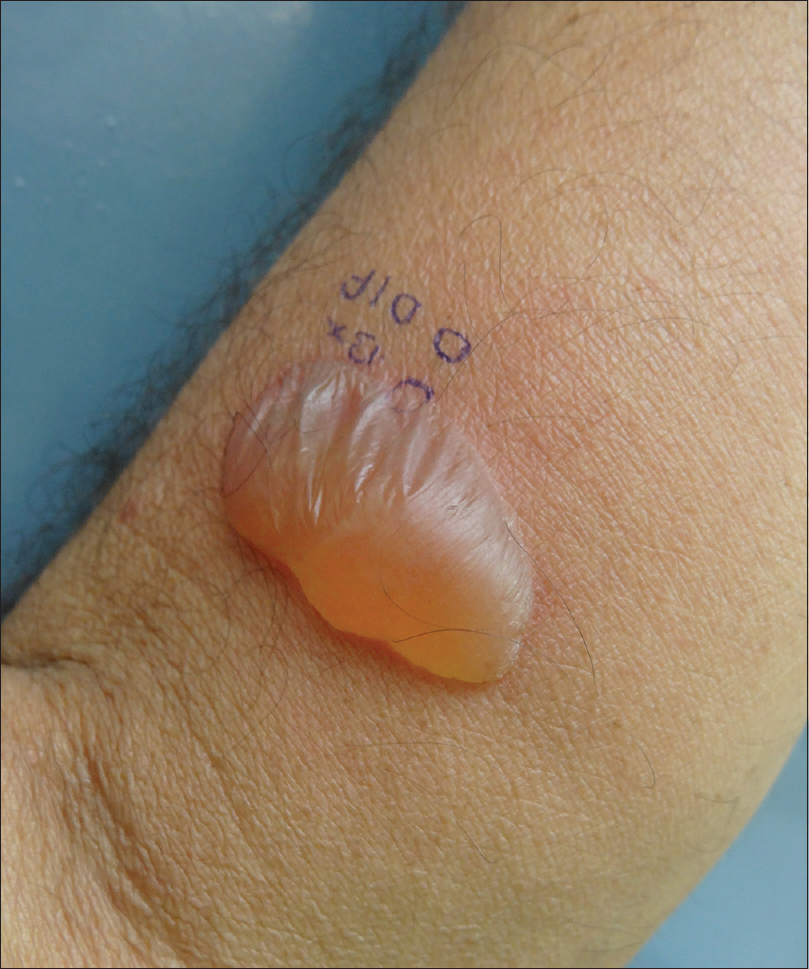 |
| Figure 1b: Close-up of the lesion |
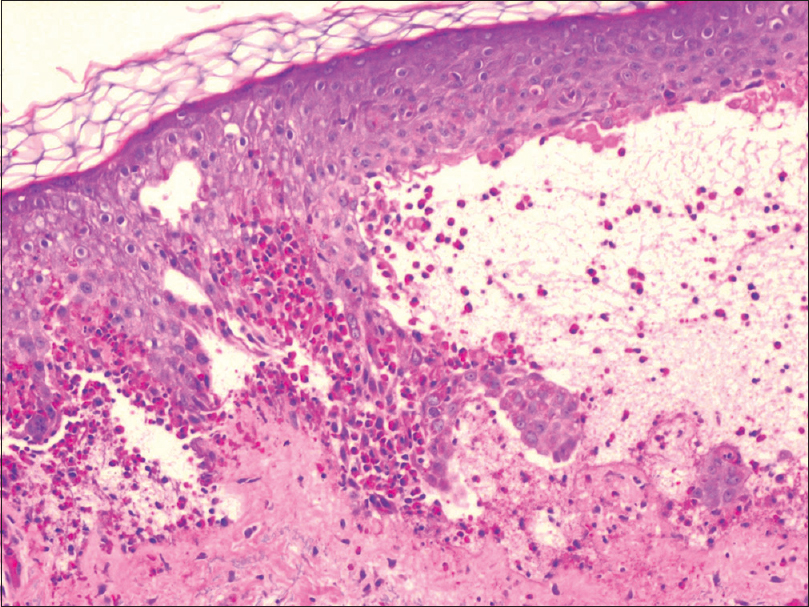 |
| Figure 2a: Subepidermal split is visible and blister cavity has numerous eosinophils and neutrophils (H and E, original magnification ×100) |
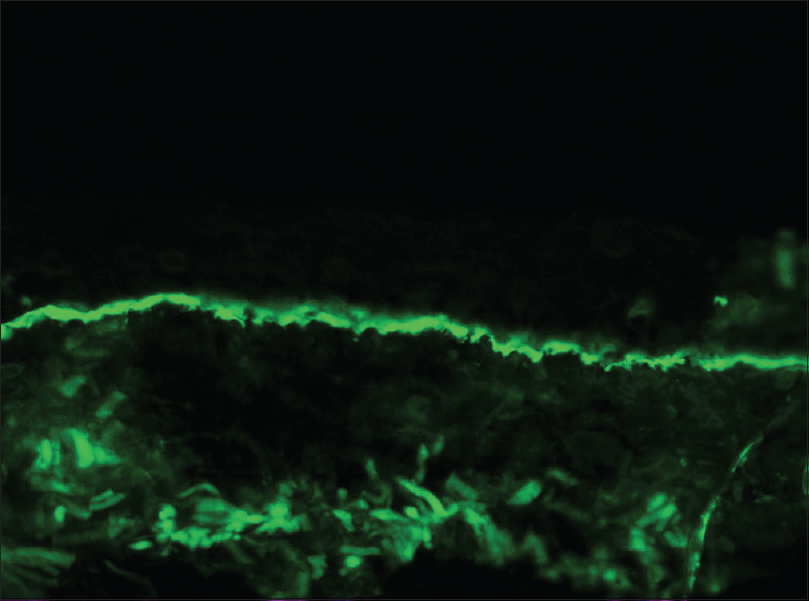 |
| Figure 2b: On direct immunofluorescence, granular deposition of immunoglobulin G is visible at the dermoepidermal junction in a linear fashion (FITC, original magnification ×100) |
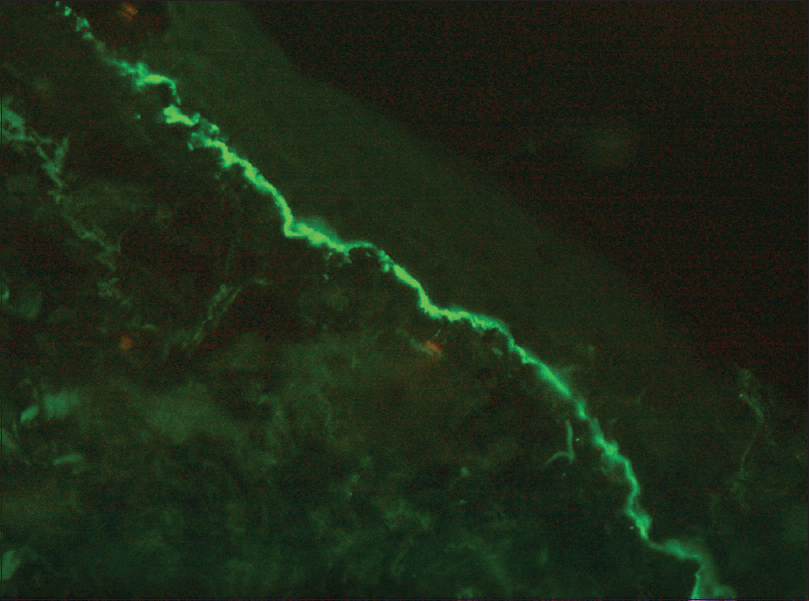 |
| Figure 2c: On direct immunofluorescence, granular deposition of complement C3 is visible at the dermoepidermal junction in a linear fashion. (FITC, original magnification ×100) |
Koebner's phenomenon has been classically described with psoriasis, lichen planus, and vitiligo.[1] Koebner's phenomenon described in autoimmune vesiculobullous diseases has been classified as questionable in view of isolated and rare case reports.[1] It has been previously described in pemphigus vulgaris [2] and pemphigus foliaceous.[3] It has been postulated that trauma leads to exposure of autoantigens with subsequent antibody-mediated response and bulla formation. There are reports of generalized bullous pemphigoid occurring after orthopedic surgery and radiotherapy with onset of disease at the the site of surgery or irradiation, respectively. Bullous pemphigoid arising at the site of vein–graft harvest on the legs has also been described.[4]
Pemphigus vulgaris koebnerizing at the site of tuberculin skin test site has been reported previously.[5] The authors proposed that the local inflammatory milieu produced by intradermal injection of purified protein derivative (interleukin-1α, interleukin-1β, tumor necrosis factorα) at 72 hours is similar to that occurring naturally in the pathogenesis of autoimmune blistering disorders. These cytokines prime a patient having autoantibodies to develop blistering at tuberculin skin test site. Our patient did not develop bullous pemphigoid lesions at venepuncture sites. The development of bullous pemphigoid lesion at tuberculin skin test site but not at other trauma sites supports the possible role of purified protein derivative in inciting this koebnerization. We were unable to find any previous reports of bullous pemphigoid koebnerizing at the tuberculin skin test site.
It is of utmost importance to identify this phenomenon and differentiate it from bullous reaction at tuberculin skin test site resulting from severe type IV hypersensitivity to purified protein derivative. The latter may represent latent tubercular infection and warrants antitubercular treatment, whereas bullous reaction resulting from koebnerization of autoimmune vesiculobullous dermatosis represents active disease, and in turn, requires treatment with immunosuppressive agents. Correct identification will help in proper patient management. [Table - 1] enlists salient points to differentiate between koebnerizing autoimmune bullous dermatosis and bullous type IV hypersensitivity reaction to purified protein derivative.

Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
| 1. |
Boyd AS, Neldner KH. The isomorphic response of Koebner. Int J Dermatol 1990;29:401-10.
[Google Scholar]
|
| 2. |
Cerottini JP, Burren R, Panizzon RG. Pemphigus vulgaris occurring simultaneously on a recent and an old surgical scar due to a koebner's phenomenon. Eur J Dermatol 2000;10:546-7.
[Google Scholar]
|
| 3. |
Rotunda AM, Bhupathy AR, Dye R, Soriano TT. Pemphigus foliaceus masquerading as postoperative wound infection: Report of a case and review of the koebner and related phenomenon following surgical procedures. Dermatol Surg 2005;31:226-31.
[Google Scholar]
|
| 4. |
Murphy B, Walsh M, McKenna K. Bullous pemphigoid arising in lower leg vein graft incision site. J Card Surg 2016;31:57-9.
[Google Scholar]
|
| 5. |
Vinay K, Kanwar AJ, Saikia UN. Pemphigus occurring at tuberculin injection site: Role of cytokines in acantholysis. Indian J Dermatol Venereol Leprol 2013;79:539-41.
[Google Scholar]
|
Fulltext Views
3,258
PDF downloads
950





