Translate this page into:
Intralesional 5-fluorouracil: Novel therapy for extensive molluscum contagiosum in an immunocompetent adult
2 Department of Medicine, Grant Government Medical College and Sir Jamshedjee Jeejeebhoy Group of Hospitals, Mumbai, Maharashtra, India
Correspondence Address:
Jinal Lakhamshi Gada
502, Shweta Saroj, Gaothan Road No. 1, Chembur, Mumbai - 400 071, Maharashtra
India
| How to cite this article: Viswanath V, Shah RJ, Gada JL. Intralesional 5-fluorouracil: Novel therapy for extensive molluscum contagiosum in an immunocompetent adult. Indian J Dermatol Venereol Leprol 2017;83:265-266 |
Sir,
Recalcitrant and/or extensive molluscum contagiosum is known to occur in immunocompromised patients. We report a case of extensive, recalcitrant molluscum contagiosum in an immunocompetent patient who responded to intralesional 5-fluorouracil.
A 65-year-old woman presented with multiple, asymptomatic, umbilicated, skin-colored papules and nodules around the right eye for 7 months. Similar lesions appeared gradually on the rest of the face, arms and the scalp. The lesions were coalescent, varying in size from 0.5 to 3 cm and had led to complete obstruction of the right eye and near-complete obstruction of the left eye. Phthisis bulbi of the right eye and trichiasis of the lids of both eyes was noted [Figure - 1]. She had no history suggestive of immunosuppression such as chronic diarrhea, recurrent chest infection, weight loss or oral ulceration. There was no history of high-risk sexual exposure or blood transfusion. There were no similar complaints in the past or in other family members. She was a known case of hypertension on treatment. Differential diagnoses of giant molluscum contagiosum, cryptococcosis and keratoacanthoma was considered. Biopsy revealed marked acanthosis with intracytoplasmic inclusion bodies suggestive of molluscum contagiosum. A detailed workup was performed to check for any immunosuppression or malignancy. All routine investigations including complete hemogram, liver, renal and thyroid function tests, blood sugars and lipid profile were normal, except for low hemoglobin of 9.4 g%. She was tested for human immunodeficiency virus by enzyme-linked immunosorbent assay on three different occasions and was found to be negative. A detailed radiological examination including a chest X-ray and ultrasonography of the abdomen and pelvis revealed no significant abnormality.
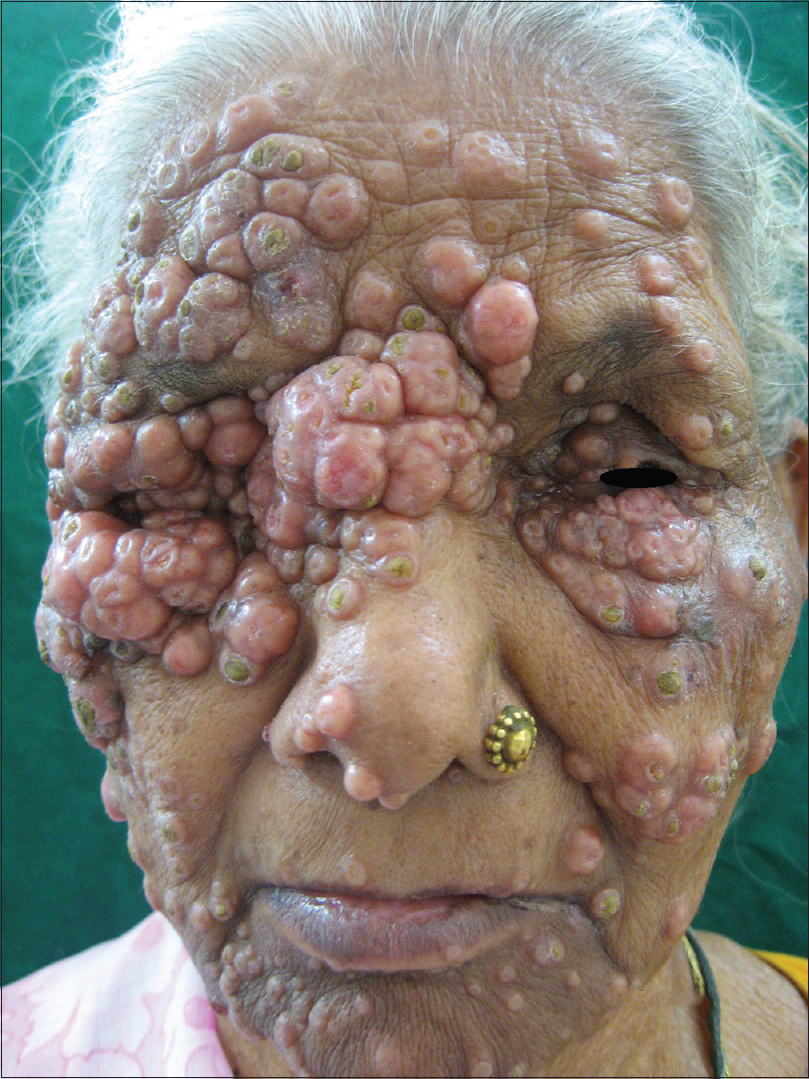 |
| Figure 1: Multiple umbilicated papules, coalescing in nature, completely obstructing the right eye |
An initial course of levamisole, 150 mg 2 tablets twice a week along with elemental zinc 50 mg/day for 6 weeks and topical 10% potassium hydroxide showed no response. Three sessions of cryotherapy with liquid nitrogen led to minimal response. Intralesional 5-flurouracil (50 mg/ml) was then administered. The lesions were pricked with a 26-gauge needle and 1-2 drops (3-6 mg) of the drug were instilled into the puncture site. The maximum dose in one session was 100 mg. Treatment was given at weekly intervals for 6 weeks. An initial inflammatory reaction followed by resolution was seen after the second session. The lesions healed with scarring within 2 months of initiation of intralesional 5-fluorouracil [Figure - 2]. An excellent response was achieved with complete resolution and no recurrence was noted during 1 year of follow-up.
 |
| Figure 2: Complete resolution of the lesions with scarring |
Molluscum contagiosum is caused by a deoxyribonucleic acid virus from the poxvirus family. Classical molluscum contagiosum is commonly seen in children. Giant molluscum, atypical presentations, uncommon locations or disseminated lesions may pose diagnostic difficulties and are frequently reported in human immunodeficiency virus-positive patients, atopic dermatitis, malignancies or in patients on immunosuppressive drugs. Histopathological examination is helpful in the diagnosis of atypical clinical presentations. Unusual presentations of molluscum contagiosum in immunocompetent individuals without any underlying skin condition or systemic disease are infrequently reported.[1] These manifest as localized lesions or giant molluscum and may herald an underlying immunodeficiency.[1],[2] A case of giant molluscum located on the scalp in a 64-year-old immunocompetent man has been reported and the atypical manifestation has been attributed to the decline in immune function in old age.[3] With advancing age, B- and T-lymphocytes have shown a reduced response to certain viral infections and contribute to atypical manifestations.[3] This factor could also explain the extensive, recalcitrant lesions in our patient.
Optimal therapy is based on the type of patient being treated. Various modalities of treatment have been described and include evisceration, curettage, tape stripping, cryosurgery, podophyllin and podofilox, cantharidin, iodine solution, salicylic acid plaster, tretinoin, cimetidine, potassium hydroxide, 5% imiquimod cream, cidofovir, interferon-alpha, candida antigen and pulsed dye laser.[4] In extensive lesions with immunodeficiency, treatment options include potassium hydroxide, 5% imiquimod cream, cidofovir and interferon-alpha.[4] Treating the underlying cause is beneficial; for example, clearance of the molluscum lesions is often noted after initiation of antiretroviral therapy in patients with human immunodeficiency virus infection. Good response to etretinate therapy has also been reported in a case with eruptive onset of molluscum contagiosum with no underlying immunodeficiency.[5] Intralesional 5-fluorouracil has been found to be an effective regimen in the treatment of hypertrophic scars and keloid and the side effects of therapy include pain, erythema, hyperpigmentation and ulceration. The drug is an antimetabolite with a cytotoxic action and also has an immunostimulatory mechanism. This mechanism could explain its efficacy in cytoproliferative viral infections such as recalcitrant warts.[6] We were unable to find any previous reports of the use of intralesional 5-fluorouracil as a cytotoxic agent in extensive, recalcitrant molluscum contagiosum in an immunocompetent patient.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient has given her consent for her images and other clinical information to be reported in the journal. The patient understands that her name and initials will not be published and due efforts will be made to conceal her identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
| 1. |
Al-Mutairi N. Unusual presentations of molluscum contagiosum. J Cutan Med Surg 2008;12:295-8.
[Google Scholar]
|
| 2. |
Matsuda M, Bloch LD, Arnone M, Vasconcelos Dde M, Nico MM. Giant molluscum contagiosum: Does it affect truly immunocompetent individuals? Acta Derm Venereol 2005;85:88-9.
[Google Scholar]
|
| 3. |
Kim HK, Jang WS, Kim BJ, Kim MN. Rare manifestation of giant molluscum contagiosum on the scalp in old age. Ann Dermatol 2013;25:109-10.
[Google Scholar]
|
| 4. |
Nguyen HP, Franz E, Stiegel KR, Hsu S, Tyring SK. Treatment of molluscum contagiosum in adult, pediatric, and immunodeficient populations. J Cutan Med Surg 2014;18:299-306.
[Google Scholar]
|
| 5. |
Singal A, Gandhi V, Bhattacharya SN, Khanna G, Baruah MC. Eruptive mollusca contagiosa in an immunocompetent Indian adult. Indian J Dermatol Venereol Leprol 1998;64:301-2.
[Google Scholar]
|
| 6. |
Isçimen A, Aydemir EH, Göksügür N, Engin B. Intralesional 5-fluorouracil, lidocaine and epinephrine mixture for the treatment of verrucae: A prospective placebo-controlled, single-blind randomized study. J Eur Acad Dermatol Venereol 2004;18:455-8.
[Google Scholar]
|
Fulltext Views
3,880
PDF downloads
885





