Translate this page into:
LEOPARD syndrome and multiple granular cell tumors: An underreported association?
2 Department of Pathology, General Universitario Gregorio Marañón, Madrid, Spain
3 Department of Biochemistry, Molecular Diagnostics Laboratory, Biomedical Investigation Institute, Hospital General Universitario Gregorio Marañón, Madrid, Spain
Correspondence Address:
Ignacio Hern�ndez Arag��s
Calle del Dr. Esquerdo, 46, 28007 Madrid
Spain
| How to cite this article: Arag��s IH, Dom�nguez MC, Blanco VP, Zubicaray BE, Fern�ndez RS. LEOPARD syndrome and multiple granular cell tumors: An underreported association?. Indian J Dermatol Venereol Leprol 2016;82:77-79 |
Sir,
A 15-year-old girl presented for the evaluation of pigmented lesions which had been progressively appearing for the last 7 years [Figure - 1]. Her mother, uncle, grandmother and brothers also had similar multiple pigmented lesions [Figure - 2].
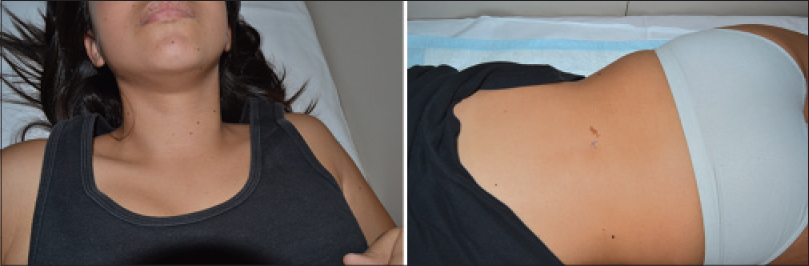 |
| Figure 1: Multiple lentigines and café au lait macules on the trunk of the patient |
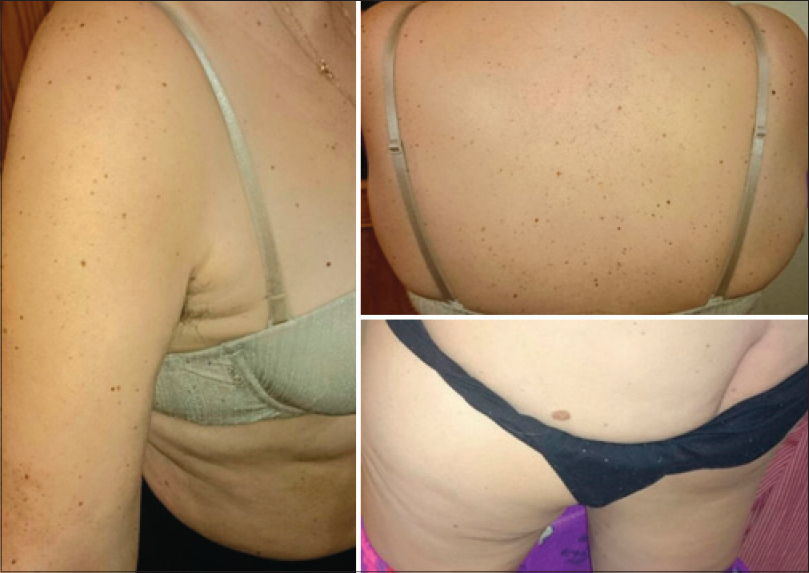 |
| Figure 2: Multiples lentigines in patient's mother. In addition, there is a café-au-lait macule on the left lumbar area |
Clinical examination revealed multiple lentigines and café au lait macules scattered over her trunk, neck and face. In addition, there was mild facial dysmorphia including hypertelorism, low-set ears and broad nasal bridge. Her mother showed a similar facial appearance and a larger number of lentigines on her trunk and face. An electrocardiogram was performed and no alterations were detected.
The patient also had a history of two subcutaneous nodules on her right foot and left arm which had been excised at the age of 10 and 11 years, respectively. Histologic study of these nodules had demonstrated nests of S100/vimentin positive cells with granular cytoplasm and small hyperchromatic nuclei with a diagnosis of granular cell tumor in both cases [Figure - 3].
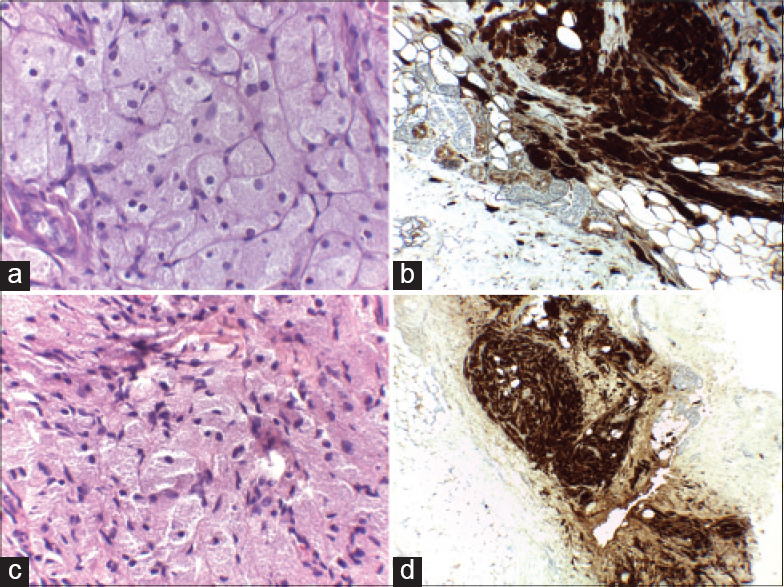 |
| Figure 3: Nests of cells with granular cytoplasm and small hyperchromatic nuclei (H and E, ×400) (a and c). Positive stain for S100 (b and d) |
In view of these clinical signs, there was clinical suspicion of a RASopathy. Genetic testing revealed a p. Gln510Arg PTPN11 mutation in the patient and in her mother. This mutation has been previously described and therefore, a diagnosis of LEOPARD (lentigenes, electrocardiographic conduction anomalies, ocular hypertelorism, pulmonary stenosis, abnormalities of genitalia, retardation of growth, deafness) syndrome was made.
Granular cell tumors are rare, generally benign neoplasms most likely of Schwann cell origin. They usually present as an asymptomatic, solitary, skin-colored nodule or papule in cutaneous and subcutaneous tissue (43%), tongue (23%) or internal organs.[1] These tumors have an excellent prognosis and the treatment of choice is surgical excision with wide margins to prevent recurrence. The characteristic histopathology shows irregularly arranged sheets of polyhedral cells with central hyperchromatic nuclei and coarse granular eosinophilic cytoplasm. These granular cells stain positive for S100 (98–100%), neuron specific enolase (98–100%) and vimentin (100%). Multiple granular cell tumors have been reported in up to 30% of cases but they are infrequent in childhood. In up to 50% of children with multiple granular cell tumors, there are asssociated systemic abnormalities such as cardiovascular, musculoskeletal and pigmentary disorders.[2]
Several cases of multiple granular cell tumors in association with neuro-cardio-facial-cutaneous syndromes have been described such as Noonan syndrome and neurofibromatosis type 1. We were able to find only two previous reports of multiple granular cell tumors reported in association with LEOPARD syndrome. The first report described a woman with confirmed LEOPARD syndrome with a c. 1403C. Tin mutation of PTPN11 gene who developed 16 nodules on the skin and subcutaneous tissue during adolescence; these nodules were histopathologically consistent with granular cell tumors and expressed S100 antigen.[3] The other reported case was a 14-year-old girl with confirmed LEOPARD syndrome due to a PTPN11 mutation. This patient presented multiple tender dermal nodules on her arms which were compatible with granular cell tumors and stained strongly positive for S100 protein.[4] Tomson et al., reviewed all cases of multiple granular cell tumors associated with systemic alterations that had been reported up to 2006.[5] They found 12 children who showed co-existing abnormalities, such as axillary freckling, café au lait spots, diffuse lentiginosis and growth retardation. The presence of lentiginosis with other typical abnormalities of LEOPARD syndrome in six patients of this case series suggests that they may represent undiagnosed cases of an association of LEOPARD syndrome and multiple granular cell tumors.
LEOPARD syndrome is caused in 85% of patients by a heterozygous missense mutation in the PTPN11 gene leading to reduced SHP2 phosphatase activity. Given the implication of germline, RAS-mitogen activated protein kinase mutations in rasopathies and tumorigenesis, the link between LEOPARD syndrome and multiple granular cell tumors could be explained by gene mutation within this signaling pathway.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
| 1. |
Torrijos-Aguilar A, Alegre-de Miquel V, Pitarch-Bort G, Mercader-García P, Fortea-Baixauli JM. Cutaneous granular cell tumor: A clinical and pathologic analysis of 34 cases. Actas Dermosifiliogr 2009;100:126-32.
[Google Scholar]
|
| 2. |
García-Bracamonte B, Fuertes L, Llamas R, Vanaclocha F. Multiple cutaneous granular cell tumors. Actas Dermosifiliogr 2010;101:732-4.
[Google Scholar]
|
| 3. |
Schrader KA, Nelson TN, De Luca A, Huntsman DG, McGillivray BC. Multiple granular cell tumors are an associated feature of LEOPARD syndrome caused by mutation in PTPN11. Clin Genet 2009;75:185-9.
[Google Scholar]
|
| 4. |
Gunson TH, Hashim N, Sharpe GR. Generalized lentiginosis, short stature, and multiple cutaneous nodules – Quiz case. LEOPARD syndrome (LS) associated with multiple granular cell tumors (GCTs). Arch Dermatol 2010;146:337-42.
[Google Scholar]
|
| 5. |
Tomson N, Abdullah A, Tan CY. Multiple granular cell tumors in a child with growth retardation. Report of a case and review of the literature. Int J Dermatol 2006;45:1358-61.
[Google Scholar]
|
Fulltext Views
2,257
PDF downloads
842





