Translate this page into:
Periocular granuloma annulare in a child
2 Department of Ophthalmology, Prabha Eye Clinic, Bengaluru, Karnataka, India
3 Department of Pathology, St. Theresa's Hospital, Bengaluru, Karnataka, India
Correspondence Address:
Sahana M Srinivas
Department of Pediatric Dermatology, Indira Gandhi Institute of Child Health, Bengaluru, Karnataka
India
| How to cite this article: Srinivas SM, Goswami M, Naik M. Periocular granuloma annulare in a child. Indian J Dermatol Venereol Leprol 2014;80:171-172 |
Sir,
Granuloma annulare is a benign, inflammatory disorder of the dermis and/or subcutis characterized by degeneration of connective tissue surrounded by lymphocytes and histiocytes. It can occur at any age but is more commonly seen in children and young adults. Characteristically, there are asymptomatic, skin colored firm, papules or plaques in an annular pattern on the trunk and extremities. [1] It is rare in the periocular region where nodules with a predilection for upper eyelids have been reported. We found 14 previously published cases of pediatric periocular granuloma, but none from India.
An 8-year-old boy was referred by the ophthalmologist for evaluation of asymptomatic, recurrent papules and nodules on both upper eyelids and eyebrows for 4 years. The lesions first appeared on the lateral brow at the age of 4 years, spontaneously disappeared in a few months and recurred at multiple sites. Cutaneous examination revealed multiple, non-tender, mobile, skin colored nodules measuring 3-5 mm located on both upper eyelids, medial and lateral canthi and the left eyebrow [Figure - 1]. Ophthalmological examination was normal. Skin biopsy from the lateral canthus showed a normal epidermis with mild interstitial and perivascular lymphocytic infiltrates. A palisade of histiocytes and lymphocytes was seen surrounding a large area of mucin in the middle and deep dermis [Figure - 2]a and b. The lesions resolved without treatment within 2 weeks [Figure - 3].
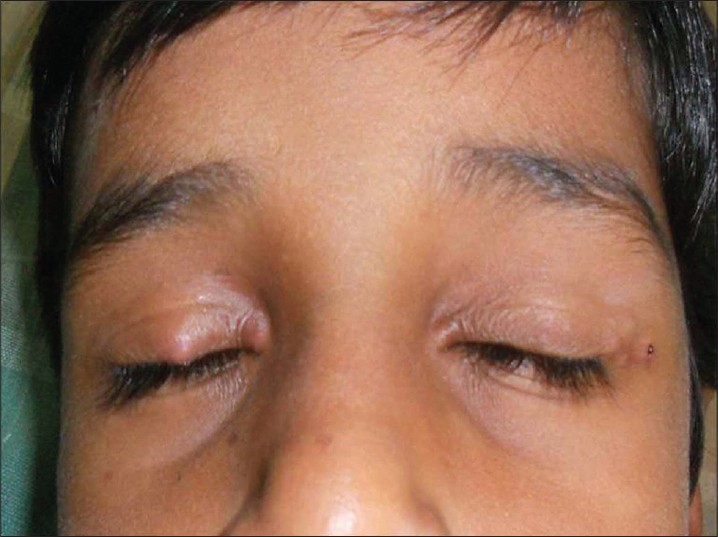 |
| Figure 1: Multiple nodules on both upper eyelids, medial and lateral canthus |
 |
| Figure 2: (a) Normal epidermis with an area showing mucin in the deep dermis (H and E, ×40), (b) Higher magnifi cation showing mucin deposition surrounded by a palisade of histiocytes and a few lymphocytes (H and E, ×400) |
 |
| Figure 3: Nodules have resolved on left upper eyelid and lateral canthus |
Localized, generalized, subcutaneous and perforating granuloma annulare are the most common variants of the condition while periocular granuloma annulare is quite rare. [2] Firm, skin-colored nodules similar to rheumatoid nodules are seen in the periocular region and some case reports refer to these lesions as "pseudorheumatoid nodules," although they are not related to rheumatoid arthritis. [3] Though the etiology of granuloma annulare is not known, implicated trigger factors include local trauma, sun exposure, cutaneous infections, insect bites, diabetes, tuberculosis, sarcoidosis and hereditary predisposition.
The age of onset in previous reports of pediatric periocular granuloma annulare ranged from 1 year to 17 years and there was no sex predilection. Most patients were African American. No co-morbidities were reported in any children. [4] Differential diagnoses include eyelid lesions such as chalazion, lupus miliaris disseminatus faciei, tuberculosis, sarcoidosis, childhood granulomatous periorificial dermatitis and granulomatous infectious processes. [5] Periocular granuloma annulare regresses spontaneously without treatment. Therapeutic interventions need to be considered only if there is functional visual impairment. Recurrences vary from 15% to 40% and regular follow-up is necessary. Parents should be counseled about the uneventful natural course of the disease to allay anxiety.
| 1. |
Cronquist SD, Stashower ME, Benson PM. Deep dermal granuloma annulare presenting as an eyelid tumor in a child, with review of pediatric eyelid lesions. Pediatr Dermatol 1999;16:377-80.
[Google Scholar]
|
| 2. |
De Becker I, Summers CG, Kaye V, Traboulsi EI, Schoenfield L, Markowitz G, et al. Periocular granuloma annulare in four children. J AAPOS 2010;14:280-2.
[Google Scholar]
|
| 3. |
Burnstine MA, Headington JT, Reifler DM, Oestreicher JH, Elner VM. Periocular granuloma annulare, nodular type. Occurrence in late middle age. Arch Ophthalmol 1994;112:1590-3.
[Google Scholar]
|
| 4. |
Chiang K, Bhalla R, Mesinkovska NA, Piliang MP, Tamburro JE. Periocular granuloma annulare: A case report and review of literature. Pediatr Dermatol 2013; [In Press].
[Google Scholar]
|
| 5. |
Goldstein SM, Douglas RS, Binenbaum G, Katowitz JA. Paediatric periocular granuloma annulare. Acta Ophthalmol Scand 2003;81:90-1.
[Google Scholar]
|
Fulltext Views
2,004
PDF downloads
771





