Translate this page into:
A case of Frey's syndrome
Correspondence Address:
Duriye Deniz Demirseren
Ataturk Training and Research Hospital, Dermatology Clinic, Ankara
Turkey
| How to cite this article: Demirseren DD, Akoglu G, Emre S, Metin A. A case of Frey's syndrome. Indian J Dermatol Venereol Leprol 2014;80:88-89 |
Sir,
Frey′s syndrome is characterized by episodic flushing, paraesthesia, and hyperhidrosis in the preauricular region. Frey′s syndrome emerges 3-24 months after surgery involving the parotid or temporo-mandibular joint. [1],[2] This syndrome may also develop due to auriculo-temporal nerve injury in patients who underwent closed treatment for maxillo-mandibular joint trauma. In the recovery process, misdirected regeneration of sympathetic nerve fibers innervating vessels and parasympathetic nerves innervating salivary glands was suggested to be involved in the pathogenesis of Frey′s syndrome. [3] Herein, we describe a female patient who developed Frey′s syndrome after mandibular surgery following a bicycle accident. This case report demonstrates a localized gustatory hyperhidrosis on the right zygomatico-facial nerve distribution, which is an unusual presentation of Frey′s syndrome.
A 38-year-old female patient presented with episodic flushing, burning sensation, and sweating on her right cheek after eating especially spicy and sour food. She did not remember exactly when these complaints had begun; however, she had a history of a bicycle accident and open surgery due to mandibular condyle fracture. Dermatological examination revealed a rapid onset of diffuse erythema on the right cheek after she ate lemon. Minor′s iodine starch test demonstrated a localized hyperhidrosis on the periorbital area over the right zygomatic arch [Figure - 1]. The right mandibular condyle was smaller than the left one on the panaromic chin radiograph. Based on these findings, the patient was diagnosed as having Frey′s syndrome.
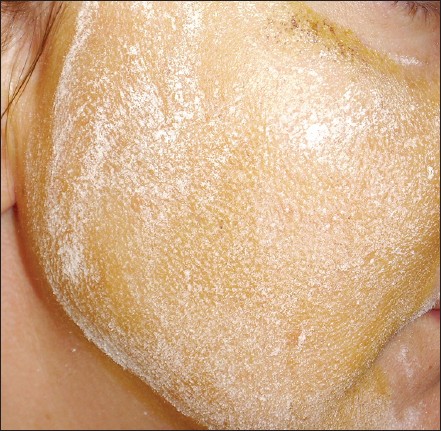 |
| Figure 1: Positive iodine starch test: gustatory hyperhidrosis became visible on the distribution of zigomaticofacial nerves |
Frey′s syndrome, which is also known as auriculo temporal syndrome or gustatory hyperhidrosis, was first described by a neurologist named Lucie Frey in 1923. [4] About 2.6%-97.6% of patients who undergo parotid surgery may have this syndrome, and severe symptoms may be observed in about 15% of them. [1],[5] The etiopathogenesis of Frey′s syndrome was suggested to involve misdirected nervous regeneration. The auriculo temporal nerve is a mixed nerve consisting of both sympathetic and parasympathetic fibers. Nerve fibers innerving salivary glands may be cut during surgery or after trauma. During the regeneration of parasympathetic nerve, a misconnection with distal sympathetic nerves of subcutaneous sweat glands was suggested to lead to development of new reflex arcs. Frey′s syndrome is diagnosed depending on the history, symptoms, and assessment with Minor′s iodine starch test. [1] Treatment choices include surgery, application of topical and systemic anticholinergic agents, antiperspirants, and botulinum toxin injections. [1],[5] In our case, the patient had a diffuse flushing on the whole cheek but only a localized hyperhidrosis over the zygomatico-facial area. To the best of our knowledge, there is no similar case with Frey′s syndrome presenting with these unique features. We cannot conclude the exact cause for our case since both trauma resulting in condylar fracture and management with surgical operation might have resulted in Frey′s syndrome. We suggest that a misdirected regeneration process might have developed to an aberrant anasotmosis between the auriculo-temporal nerve and the zygomatico-facial branch of the maxillary nerve innerving sweat glands.
| 1. |
Rustemeyer J, Eufinger H, Bremerich A. The incidence of Frey�s syndrome. J CraniomaxillofacSurg 2008;36:34-7.
[Google Scholar]
|
| 2. |
Mellor TK, Shaw RJ. Frey�s syndrome following fracture of the mandibular condyle: Case report and literature review. Ýnjury 1996;27:359-60.
[Google Scholar]
|
| 3. |
Kragstrup TW, Christensen J, Fejerskov K, Wenzel A. Frey syndrome-an underreported complication to closed treatment of mandibular condyle fracture? Case report and literature review. J Oral Maxillofac Surg 2011;69:2211-6.
[Google Scholar]
|
| 4. |
Frey L. Le syndrome du nerf auriculo-temporal. Rev Neurol 1923;2:97-104.
[Google Scholar]
|
| 5. |
Sverzut CE, Trivellato AE, Serra EC, Ferraz EP, Sverzut AT. Frey's syndrome after condylar fracture: Case report. Braz Dent J 2004;15:159-62.
[Google Scholar]
|
Fulltext Views
2,643
PDF downloads
1,664





