Translate this page into:
Prevalence and clinical patterns of psoriatic arthritis in Indian patients with psoriasis
2 Department of Internal Medicine, Division of Rheumatology and HIV, Postgraduate Institute of Medical Education and Research, Chandigarh, India
Correspondence Address:
Sunil Dogra
Department of Dermatology, Venereology and Leprology, Postgraduate Institute of Medical Education and Research, Chandigarh - 160 012
India
| How to cite this article: Kumar R, Sharma A, Dogra S. Prevalence and clinical patterns of psoriatic arthritis in Indian patients with psoriasis. Indian J Dermatol Venereol Leprol 2014;80:15-23 |
Abstract
Background: The prevalence and clinical patterns of psoriatic arthritis (PsA) varies in different parts of the world and there is little clinical and epidemiological data from the Indian subcontinent. Aims: Our study was designed to evaluate the prevalence and clinical patterns of PsA in Indian patients. Methods: This was a non-interventional, cross-sectional study, in which 1149 consecutive psoriasis patients seen over 1 year were screened for PsA according to classification of psoriatic arthritis (CASPAR) criteria. Demographic and disease parameters were recorded including Psoriasis Area and Severity Index (PASI), Nail Psoriasis Severity Index (NAPSI), and number of swollen and tender joints. Results: Among 1149 patients with psoriasis, 100 (8.7%) patients had PsA, of which 83% were newly diagnosed. The most common pattern was symmetrical polyarthritis (58%), followed by spondyloarthropathy 49%, asymmetric oligoarthritis (21%), isolated spondyloarthropathy (5%), predominant distal interphalangeal arthritis (3%), and arthritis mutilans (1%). Enthesitis and dactylitis were present in 67% and 26% of cases, respectively. The mean number of swollen and tender joints were 3.63 ± 3.59 (range, 0-22) and 7.76 ± 6.03 (range, 1-26), respectively. Nail changes were present in 87% of the cases. The median PASI and NAPSI of the subjects with PsA was 3.6 and 20, respectively. There was no significant correlation of number of swollen/tender joints with PASI or NAPSI. Conclusion: There is a relatively low prevalence of PsA among Indian psoriasis patients presenting to dermatologists. No correlation was found between the severity of skin and nail involvement and articular disease.Introduction
Psoriatic arthritis (PsA) has been defined as an inflammatory arthritis associated with psoriasis, usually seronegative for rheumatoid factor (RF). [1] The data on prevalence of PsA among patients of the psoriasis varies from 6.25% to 48% in western countries. [2],[3] A relatively low figures are reported from Asian countries such as Korea (9%), [4] Iran (9%), [5] China (5.8%), [6] Turkey (2%, [7] and Japan (1%). [8] In a small series from South India PsA was reported in 8.47% cases of psoriasis. [9]
The heterogeneity of the prevalence and clinical forms of PsA is variable and can result in a progressive and mutilating course if not managed effectively. The most frequently used PsA clasification has been Moll and Wright′s classification [1] whereas the recently proposed classification of psoriatic arthritis (CASPAR) [10] criteria are simple and highly specific.
Several large series have been published about characteristics of skin involvement in psoriasis, but comprehensive data about prevalence and morbidity of PsA are still lacking in the Indian subcontinent. It is perhaps underdiagnosed in Indian settings or may be confused or misdiagnosed with other rheumatological diseases such as rheumatoid arthritis and osteoarthritis. To provide optimal therapy to all patients of PsA and for policy making, it is important to know the prevalence, clinical patterns, burden of disease, and economic considerations in a given geographical population. In this study, we analyzed the prevalence and clinical patterns of PsA in our patient population of psoriasis.
Study population and methods
Study design
This was a non-interventional, cross-sectional study in which patients attending the psoriasis clinic of our centre between January 2010 and December 2010 were screened for the presence of PsA. Two dermatologists and one rheumatologist were involved in this study.
Data collection
All consecutive psoriasis patients in this study period were screened for the presence of PsA. An informed consent was taken from all the patients included in the study. Psoriasis was diagnosed clinically based on the presence of characteristic skin lesions. Demographic and disease data were recorded in a predesigned proforma including age of onset of disease, family history of psoriasis, duration of skin lesions, morphological types of psoriasis, disease variables such as "Koebner" phenomenon, aggravating/initiating factors, hospitalization due to psoriasis, presence of nail psoriasis, previous and current treatment of psoriasis (including topical therapy, phototherapy, and systemic therapy), productivity parameters such as number of work days lost in the past 12 months and the concomitant diseases . Severity of skin and nail involvement were assessed by the Psoriasis Area and Severity Index (PASI score ranges from 0 to 72, mild 0-3, moderate 3-10, and severe >10) [11] and Nail Psoriasis Severity Index respectively (total NAPSI score ranges from 0 to160). [12]
Baseline evaluation including complete hemogram (hemoglobin, total and differential leukocytes count, and platelet count), erythrocyte sedimentation rate (ESR), liver function(serum transaminases [AST, ALT], alkaline phosphatase [ALP], serum bilirubin, and serum albumin) and renal function (serum creatinine, blood urea, and serum uric acid) tests, lipid profile (total cholesterol, triglycerides, HDL, LDL, and VLDL), random blood sugar (RBS), RF, C-reactive protein (CRP), and radiography for affected joints were performed.
Diagnosis of psoriatic arthritis
Diagnosis of PsA was made on the basis of a multilevel diagnostic algorithm [Figure - 1]. In case the diagnosis of PsA had already been confirmed at a previous visit, it was documented and status of the joints was recorded.
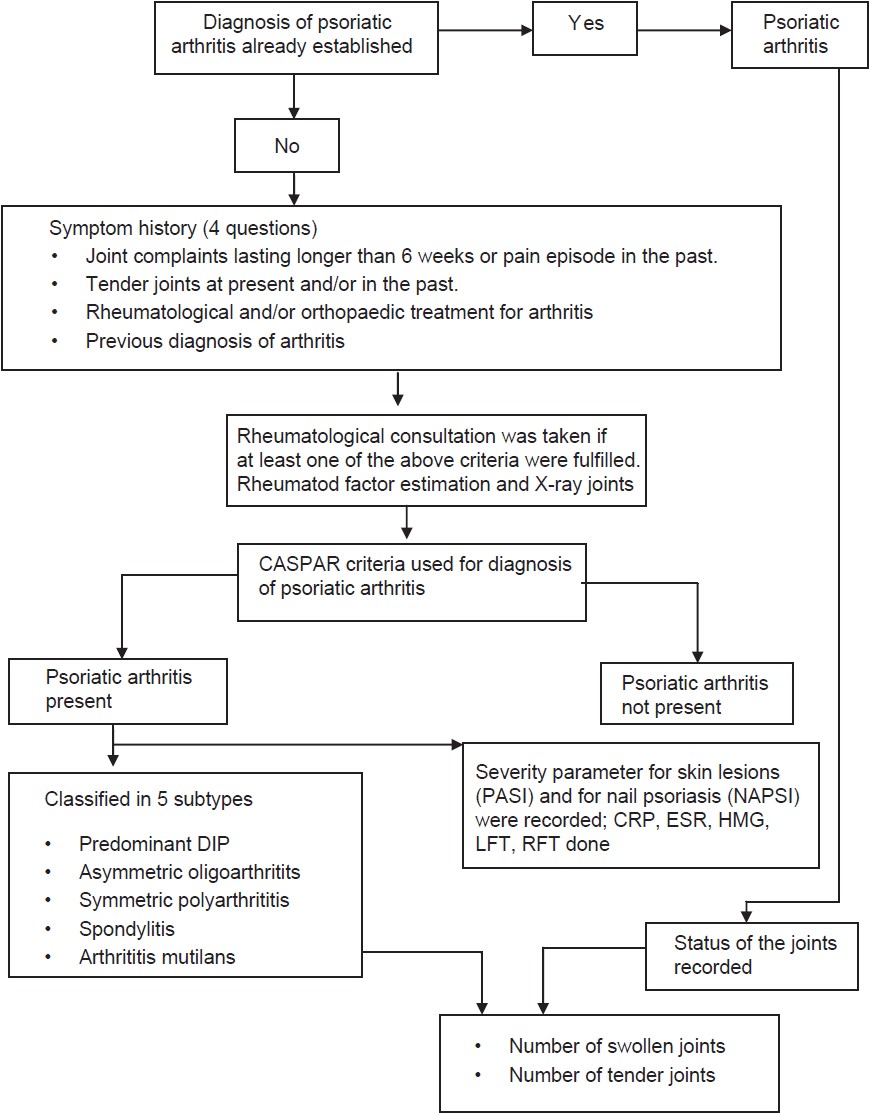 |
| Figure 1: Diagnostic algorithm for psoriatic arthritis. CASPAR: classifi cation for psoriatic arthritis; PASI: psoriasis area severity index; NAPSI: nail psoriasis severity index; DIP: distal interphalangeal |
If joint symptoms and a previously unconfirmed PsA were present, patients were examined for the presence of the following criteria indicating possible joint involvement: (1) Joint complaints lasting for longer than 6 weeks or pain episode in the past, (2) tender joints at present and/or in the past, (3) rheumatological and/or orthopedic treatment for arthritis, and (4) previous diagnosis of arthritis. If at least one of these criteria was fulfilled, rheumatology consultation was taken. During rheumatological evaluation, the presence of PsA, activity, and type of arthritis was assessed.
The diagnosis of PsA was based on the classification of psoriatic arthritis (CASPAR) [10] criteria. To meet these criteria, a patient must have established inflammatory articular disease (joint, spine, or entheseal) and a score of at least 3 based on the following categories: current psoriasis (assigned a score of 2; all other features assigned a score of 1), a history of psoriasis (unless current psoriasis was present), a family history of psoriasis (unless current psoriasis was present or there was a history of psoriasis), dactylitis, radiographic evidence of juxta-articular new bone formation, a negative test for RF, and typical nail dystrophy. In all patients with PsA, the number of tender and/or swollen joints were counted and the pattern of arthritis was recorded according to Moll and Wright′s classification criteria [3] as follows: Distal interphalangeal arthritis (DIP), asymmetric oligoarthritis (≤4 joints), symmetric polyarthritis (≥5 joints), arthritis mutilans, and arthritis of spine (spondylitis). Spondylitis was diagnosed when at least one of the following was present in a patient with inflammatory back pain, with or without peripheral joint disease:(1) Tenderness on the spine or sacroiliac joint, (2) sacroiliitis on pelvis X-ray (anteroposterior view), (3) spinal syndesmophytes on spine X-ray. The presence of enthesitis and dactylitis was diagnosed clinically and sites were recorded. Enthesitis was defined as the presence of spontaneous pain and tenderness at entheses. Enthesitis was diagnosed on clinical examination at the following sites: (a) common extensor insertion at the lateral epicondyle of humerus, (b) medial femoral epicondyle, and (c) achilles tendon insertion at calcaneus. Dactylitis was defined by the presence of spontaneous fusiform swelling and/or redness of fingers and/or toes extending beyond the joint line associated with tenderness. We managed the patients according to the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis (GRAPPA) treatment guidelines for PsA. [13]
Statistical analysis
Statistical analysis was carried out using Statistical Package for Social Sciences (SPSS Inc., Chicago, IL, version 15.0 for Windows). Normality of data was checked by measures of Kolmogorov-Smirnov tests of normality. For normally distributed data, means were compared using Student′s t-test for two groups. For skewed data, the Mann-Whitney test was applied. Qualitative or categorical variables were described as frequencies and proportions. Proportions were compared using Chi square or Fisher′s exact test whichever was applicable. For more than two groups, one-way ANOVA or Kruskal-Wallis test was applied. To see the relationship between two scores, the Spearman correlation coefficient was calculated. All statistical tests were two-sided and performed at a significance level of α =0.05.
Results
Overall, 1149 patients with psoriasis were seen over this period. Out of 1149 patients with psoriasis, 129 (11.23%) fulfilled at least one of the above criteria, which was considered indicative of possible joint involvement. In 17 of these patients, diagnosis of PsA had already been established in the past. In addition, 83 of 112 (74.1%) patients were newly diagnosed with PsA [Figure - 2]. Thus, in the entire population of patients with psoriasis, the total prevalence of PsA was 8.7% (n/N = 100/1149) with 83% of the cases being diagnosed for the first time. Patients having osteoarthritis or other diagnosis of arthritis were excluded.
 |
| Figure 2: Flowchart of patients recruited in the study |
The mean age of the study group was 42.98 ± 12.06 years (range, 16-70 years), and the male-to-female ratio was 1.7:1 (63:37). The mean age of onset of psoriasis was 33.11 ± 11.2 years (range, 2-65 years), and the mean duration of psoriasis was 9.88 ± 10.2 years (range, 8 months-46 years). The mean age of onset of PsA was 38.57 ± 11.34 years (range, 15-65 years), and the median duration of PsA was 2.5 years (range, 8 months-40 years). Family history of psoriasis was present in 16.7% and family history of PsA was present in 4% of the study group. Plaque psoriasis was the most common clinical type, observed in 95% of PsA patients, guttate in 27%, pustular in 7%, and erythroderma in 4% cases. Nail involvement due to psoriasis was present in 87% of the cases [Table - 1].

PsA occurred between 30 and 50 years in 63% of the patients. Psoriasis preceded the PsA in 70% of cases with a mean interval of 9.14 years (range, 5 months-38 years), whereas simultaneous onset of joint and skin disease was found in 17% of the patients. PsA preceded psoriasis in 13% of cases with mean interval of 4.23 years (range, 1-11 years). These patients had a history of joint involvement before skin involvement but when they presented to our psoriasis clinic, they had both skin and joint disease.
The most common pattern of PsA was symmetrical polyarthritis [Figure - 3] in 58% cases (isolated symmetrical polyarthritis in 26%, symmetrical polyarthritis with spondylitis in 32%), followed by spondyloarthropathy in 49% cases (isolated spondylitis in 5%, spondylitis + symmetrical polyarthritis in 32%, spondylitis and asymmetrical oligoarthritis in 11%, spondylitis and DIP arthritis in 1%), asymmetric oligoarthritis (21%), isolated spondyloarthropathy (5%), predominant DIP arthritis (3%), and arthritis mutilans (1%) [Figure - 4]a, b and [Figure - 5]a, b, and [Figure - 6], [Table - 2].

 |
| Figure 3: Psoriatic arthritis: symmetrical polyarthritis involving multiple distal interphalangeal joints and finger nail involvement |
 |
| Figure 4: (a) Opera glass hands in psoriatic arthritis (mutilating psoriatic arthritis). (b) Arthritis mutilans. Characteristic radiographic changes in psoriatic arthritis include erosions at several joints of hands (MCP, PIP, and DIP) with ankylosis, sclerosis, and deformity |
 |
| Figure 5: (a) Finger nail involvement and psoriatic arthritis involving interphalangeal joints of hands. (b) X-ray bilateral hands (AP view) including the wrist joint showing decreased joint space at the second, third, and fourth distal interphalangeal joints (DIP) of the right hand and fourth PIP joint and fi fth DIP joint of the left hand. There is a dislocation at the fi fth PIP joint of the left hand due to psoriatic arthritis |
 |
| Figure 6: X-ray pelvis AP view showing bilateral asymmetric sacroiliitis (right > left), with evidence of subchondral sclerosis and erosions due to psoriatic arthritis |
The most common site of involvement by psoriasis was trunk and limbs each in 70% of the cases followed by scalp (52%) and flexural sites in 40% patients. PASI of the study group was 3.6 (median, range 1-44). The severity of psoriasis according to the PASI score was mild (PASI < 3) in 42% cases, moderate (PASI 3-10) in 47% cases, and severe (PASI > 10) in 11% of the study group. There was no statistically significant correlation between the number of swollen/tender joints and PASI.
Nail changes were present in 87% of the subjects in the study group. The most common nail changes observed were pitting (59%), followed by onycholysis (54%) and subungual hyperkeratosis in 50% cases [Figure - 5]a. NAPSI of the study group was 20 (median, range 0-135). Periungual and/or nail fold psoriasis lesions were present in 15% of patients with nail involvement. There was no statistically significant correlation between the number of swollen/tender joints and NAPSI. Enthesitis and dactylitis were present in 67% and 26% of the cases, respectively. The mean number of swollen and tender joints were 3.63 ± 3.59 (range, 0-22) and 7.76 ± 6.03 (range, 1-26), respectively. The most common site of enthesitis was Achilles tendon (36%), followed by patellar tendon (27%), plantar fascia (17%), and rotator cuff in 11% of the cases.
RF was negative in all patients with PsA while the mean ESR and uric acid level were 34.86 ± 12.7 (range, 10-67 mm/h) and 4.5 ± 0.98 (range, 2.4-6.8 mg/dL), respectively. CRP was raised (>6 mg/dL) in 62% cases and abnormal x-ray finding involved joints were seen in 29% patients. The most common abnormal radiologic finding was erosions (14%), followed by sacroiliitis (12%), periosteal reaction (9%), joint space narrowing (7%), and ankylosis and sclerosis each in 5% cases.
Dicussion
Psoriasis is a chronic, inflammatory disease affecting 2-3% of the world population. [14] It accounts for 2.3% of total dermatology outpatients in India. [15] Comorbidities associated with psoriasis can be due to common pathogenetic mechanisms such as PsA and as a result of chronic inflammation due to psoriasis such as cardiovascular disorders and metabolic syndrome. [16] Now, the term "psoriatic disease" is emerging to denote the various comorbidities in patients with psoriasis. [17] The prevalence of PsA varies worldwide, ranging from 6.25% to 48% [2],[3] among psoriasis patients in Europe, North America, and South Africa, but low prevalence has been observed in Asian countries ranging from 1% to 9% among psoriasis patients. [4],[5],[6],[7],[8],[9] We found the prevalence of PsA to be 8.7% in a one year study period. The prevalence rate varies among different studies due to geographical and ethnic differences, different characteristics of the patients with psoriasis, and type of diagnostic criteria used for PsA. [18],[19] The age of onset for PsA has been reported from 30 to 50 years, a range which is similar to that of rheumatoid arthritis. [20] In our study, 63% of patients were in the age group of 30-50 years. Another Indian study [21] has reported a peak incidence (69%) of PsA in the fourth and fifth decades of life. The mean age at onset of PsA was 39.2 years (fourth decade) in Chinese population. [6] PsA affects men and women almost equally [22],[23],[24] while our study showed a male preponderance (M: F =1.7:1). Wright [25] and Jajic and el-Assadi [26] and some Indian studies [9],[27],[28] have reported similar findings while Nigam et al. [29] have reported a female preponderance . We found a male preponderance which could also be due to the overall proportion of male patients visiting the clinic being higher.
In our study, psoriasis skin lesions preceded PsA in 70 patients (70%), and in 13 patients (13%) PsA preceded skin lesions, while in 17 patients (17%) they occurred simultaneously. Similar observations have been made in various studies from other parts of the world. [6],[30] We also observed that PsA is relatively rare (80% vs. 20%) after 10 years of onset of skin lesions. This may be due to the fact that patients with long-standing psoriasis on various disease-modifying immunosuppressive agents do not display overt joint manifestations. Rajendran et al. [21] found onset of joint pain after onset of skin lesions in 50.8%, before in 12.1% and simultaneously in 37% of the cases in a rheumatology clinic setting.
The most common clinical and/or morphological type of psoriasis in our patients with PsA was chronic plaque psoriasis, noted in 95% of the patients. The most common site of involvement was trunk and limbs each in 70% of the cases followed by scalp in 52%, and flexural sites in 40% cases. Studies from different parts of the world have also reported chronic plaque type psoriasis to be the commonest manifestation, which varies from 72% to 92%. [6],[9],[22],[31] Scalp was the most common initial site of involvement in some previous studies. [6],[9],[22],[31] We observed trunk and limbs as most common initial sites of involvement. The early scalp involvement by psoriasis patients is often ignored as common dandruff.
There is a controversy about the relationship between severity of skin lesions and PsA. Some studies suggested that patients with PsA have more severe psoriasis, [6],[31] while others reported that there is no direct association between the severity of psoriasis and joint manifestations. [32],[33],[34] The median PASI of our study group was 3.6. We did not observe significantly higher PASI in our patients with PsA.
The reported frequency of nail involvement in patients with PsA varies from 63% to 97%. [9],[35],[36],[37] In our study, 87% patients with PsA had nail changes while 67% showed more than one nail finding. Nail changes in a patient with psoriasis should prompt a search for joint disease. There is a strong anatomical link between PsA and nail inflammation. [38] Enthesitis is almost always present in early DIP joint involvement in PsA and this inflammatory reaction around the DIP joint is sufficiently extensive to envelop the nail matrix. This association can be further investigated by using high-resolution magnetic resonance imaging (MRI) to detect subtle cases of PsA.
Although PsA can involve any joint, those most commonly involved are reported to be the wrists and small joints of the hands and feet. [26],[39] In our patients, however, most frequently involved joints were the hand PIPs followed by DIPs, sacroiliac, and knee joints. Many authors have demonstrated that oligoarthritis was the most common pattern of PsA, occurring in 42-67% of patients. [6],[9],[5],[40] Studies by Rajendran et al. [21] (48.3%) and Reich et al. [35] (58.3%) have reported polyarthritis as the most common pattern [Table - 3] while some other authors reported spondylitis as the predominant type occurring in 50% cases. [4],[41]

In our study, the most common pattern of PsA was polyarthritis observed in 58% cases (isolated SP in 26%, SP with SpA in 32%). Asymmetric oligoarthritis was noted in 21%, predominant DIP involvement (3%), and arthritis mutilans in 1% of cases. The most plausible explanation for symmetrical polyarthritis being the commonest pattern could be long-standing skin disease (mean, 9.88 years) in our study group. Mean number of swollen and tender joints was 3.63 ± 3.59 (range, 0-22) and 7.76 ± 6.03 (range, 1-26), respectively, in our study patients. All patients with joint swelling had associated pain and tenderness. The prevalence of different type of PsA has been found to be variable with the duration of psoriasis. With shorter disease duration, oligoarthritis [42] is prevalent whereas with longer duration polyarthritis predominates. [24],[26] Jone′s et al. noted progression of mono- or oligoarthritis to polyarticular patterns of PsA in 63% of cases over a period of 12.2 years. [33] Isolated spondylitis in PsA is uncommon and mostly occurs with peripheral arthritis. In our study also, isolated spondylitis was found in only 5% (5/100) of patients with PsA, whereas spondylitis with peripheral arthritis was found in 44% (44/100) cases. A possible explanation for such a high figure (49%) of spondylitis in our patients is a genetic predisposition for psoriatic spondyloarthropathy in Indian patients.
Dactylitis and enthesopathy are the characteristic manifestations of PsA, occurring in 16-40% and 40-45% of cases, respectively. [4],[24],[41],[42] Enthesitis is the presence of spontaneous pain and tenderness at entheses while dactylitis is the presence of spontaneous swelling and/or redness of fingers and/or toes with tenderness. In our study, enthesitis was found in 67% of cases, most commonly at the Achilles tendon insertion (36%) which is significantly higher as compared to previous studies (7.8-26.8%). [4],[6],[21],[31] This higher frequency of enthesitis in our patients could be possibly due to frequent minor trauma during work, general habit of bare foot walking, and some genetic predisposition in Indians. In our study, dactylitis was found in 26% of cases. Almost similar results were found in studies by Shah et al. [27] and Radtke et al . [31] but lower incidence has been reported in other studies [4],[6] [Table - 2].
Radiologic abnormalities were noted in 29% of our patients. The most common radiographic feature was bony erosions in 14% of the patients while 12% had findings consisted with sacroilietis. Similar observations had also been made in other studies. [24],[42] In early PsA, X-ray findings may not detect changes such as enthesitis. In 3% of PsA patients, RF can be positive but we did not find any of the case testing positive for RF. There are conflicting reports in the literature regarding the raised ESR and CRP levels in PsA patients. [24],[27],[41],[42] In our study, we found raised ESR in 88% and raised CRP in 62% of the cases. The limitation of our study was that this was a cross-sectional study with a relatively small sample size. Longitudinal follow-up of large number of patients will provide us more information regarding the changing pattern of PsA and the relationship between the site and type of skin involvement with articular disease.
Thus, we conclude that in the entire population of patients with psoriasis (1149), the total prevalence of PsA was 8.7% (n/N = 100/1149) with 83% of the cases being diagnosed for the first time. This low prevalence figures of PsA in Asian and Indian patients of psoriasis could be due to some unknown genetic factors and lack of awareness about the PsA. However, this may be an underestimate of the burden of PsA because of underreporting by patients in early/asymptomatic disease. Thus, dermatologists should ask about the joint symptoms in all psoriasis patients and screening for PsA must be done in all suspected cases of PsA for early diagnosis and intervention. Further larger epidemiological and genetic linkage studies are warranted to explain the wide variation in prevalence and patterns of disease in different populations.
| 1. |
Moll JM, Wright V. Psoriatic arthritis. Semin Arthritis Rheum 1973;3:55-78.
[Google Scholar]
|
| 2. |
Shbeeb M, Uramoto KM, Gibson LE, O'Fallon WM, Gabriel SE. The epidemiology of psoriatic arthritis in Olmsted County, Minnesota, USA, 1982-1991. J Rheumatol 2000;27:1247-50.
[Google Scholar]
|
| 3. |
Alenius GM, Stenberg B, Stenlund H, Lundblad M, Dahlqvist SR. Inflammatory joint manifestations are prevalent in psoriasis: Prevalence study of joint and axial involvement in psoriatic patients, and evaluation of a psoriatic and arthritic questionnaire. J Rheumatol 2002;29:2577-82.
[Google Scholar]
|
| 4. |
Baek HJ, Yoo CD, Shin KC, Lee YZ, Kang SW, Lee EB, et al. Spondylitis is the most common pattern of psoriatic arthritis in Korea. Rheumatol Int 2000;19:89-94.
[Google Scholar]
|
| 5. |
Jamshidi F, Bouzari N, Seirafi H, Farnaghi F, Firooz A. The prevalence of psoriatic arthritis in psoriatic patients in Tehran, Iran. Arch Iran Med 2008;11:162-5.
[Google Scholar]
|
| 6. |
Yang Q, Qu L, Tian H, Hu Y, Peng J, Yu X, et al. Prevalence and characteristics of psoriatic arthritis in Chinese patients with psoriasis. J Eur Acad Dermatol Venereol 2011;25;1409-14.
[Google Scholar]
|
| 7. |
Kundakci N, Tursen U, Babiker MO, Gurgey E. The evaluation of the sociodemographic and clinical features of Turkish psoriasis patients. Int J Dermatol 2002;41:220-4.
[Google Scholar]
|
| 8. |
Kawada A, Tezuka T, Nakamizo Y, Kimura H, Nakagawa H, Ohkido M, et al. A survey of psoriasis patients in Japan from 1982 to 2001. J Dermatol Sci 2003;31:59-64.
[Google Scholar]
|
| 9. |
Prasad PV, Bikku B, Kaviarasan PK, Senthilnathan A. A clinical study of psoriatic arthropathy. Indian J Dermatol Venereol Leprol 2007;73:166-70.
[Google Scholar]
|
| 10. |
Taylor W, Gladman D, Helliwell P, Marchesoni A, Mease P; CASPAR study group. Classification criteria for psoriatic arthritis: Development of new criteria from a large international study. Arthritis Rheum 2006;54:2665-73.
[Google Scholar]
|
| 11. |
Feldman SR. The design of clinical trials in psoriasis: Lessons from clinical practice. J Am Acad Dermatol 2003;49:62-5.
[Google Scholar]
|
| 12. |
Rich P, Richard K. Nail Psoriasis Severity Index: A usuful tool for evaluation of nail psoriasis. J Am Acad Dermatol 2003;49:206-12.
[Google Scholar]
|
| 13. |
Ritchlin CT, Kavanaugh A, Gladmann DD, Mease PJ, Helliwell P, Boehncke WH, et al. Treatment recommendations for psoriatic arthritis. Ann Rheum Dis 2009;68:1387-94.
[Google Scholar]
|
| 14. |
Naldi L, Svensson A, Diepgen T. Randomized clinical trials for psoriasis 1997-2000: The EDEN survey. J Invest Dermatol 2003;120:738-41.
[Google Scholar]
|
| 15. |
Kaur I, Handa S, Kumar B. Natural history of psoriasis: A study from Indian subcontinent. J Dermatol 1997;24:230-4.
[Google Scholar]
|
| 16. |
Christophers E. Comorbidities in psoriasis. J Eur Acad Dermatol Venereol 2006;20:52-5.
[Google Scholar]
|
| 17. |
Ritchlin C. Psoriatic disease - from skin to bone. Nat Clin Pract Rheumatol 2007;3:698-706.
[Google Scholar]
|
| 18. |
Gladman DD. Psoriatic arthritis. Baillieres Clin Rheumatol 1995;9:319-29.
[Google Scholar]
|
| 19. |
Helliwell PS, Taylor WJ. Classification and diagnostic criteria for psoriatic arthritis. Ann Rheum Dis 2005;64:3-8.
[Google Scholar]
|
| 20. |
Wilson FC, Icen M, Crowson CS, McEvoy MT, Gabriel SE, Kremers HM. Time trends in epidemiology and characteristics of psoriatic arthritis over 3 decades: A population-based study. J Rheumatol 2009;36:361-7.
[Google Scholar]
|
| 21. |
Rajendran CP, Ledge SG, Rani KP, Mahadevan R. Psoriatic arthritis. J Assoc Physicians India 2003;51:1065-8.
[Google Scholar]
|
| 22. |
Ruderman EM, Tambar S. Psoriatic arthritis: Prevalence, diagnosis, and review of therapy for the dermatologist. Dermatol Clin 2004;22:477-86.
[Google Scholar]
|
| 23. |
Aslanian FM, Lisboa FF, Iwamoto A, Carneiro SC. Clinical and epidemiological evaluation of psoriasis: Clinical variants and articular manifestations. J Eur Acad Dermatol Venereol 2005;19:141-2.
[Google Scholar]
|
| 24. |
Gladman DD, Shuckett R, Russell ML, Thorne JC, Schachter RK. Psoriatic arthritis (Psoriatic arthritis) - an analysis of 220 patients. Q J Med1987;62:127-41.
[Google Scholar]
|
| 25. |
Wright V. Psoriasis and arthritis. Ann Rheum Dis 1956;15:348-56.
[Google Scholar]
|
| 26. |
Jajic Z, el Assadi G. Prevalence of psoriatic arthritis in a population of patients with psoriasis. Acta Med Croatica 2003;57:323-6.
[Google Scholar]
|
| 27. |
Shah NM, Mangat G, Balakrishnan C, Joshi VR. Psoriatic arthritis: A study of 102 patients. J Indian Rheumat Assoc 1995;3:133-6.
[Google Scholar]
|
| 28. |
Nadkar MY, Kalgikar A, Samant RS, Borges NE. Clinical profile of psoriatic arthritis. J Indian Rheumat Assoc 2000;8:40.
[Google Scholar]
|
| 29. |
Nigam P, Anil KR, Srivasta C, Uxa AK, Mukhija RD, Jain RX. Psoriatic arthritis: A clinico-radiological study. J Indian Rheumat Assoc 1998;6:89.
[Google Scholar]
|
| 30. |
Winchester R. Psoriatic arthritis. Dermatol Clin 1995;13:779-92.
[Google Scholar]
|
| 31. |
Radtke MA, Reich K, Blome C, Rustenbach S, Augustin M. Prevalence and clinical features of psoriatic arthritis and joint complaints in 2009 patients with psoriasis: Results of a German national survey. J Eur Acad Dermatol Venereol 2009;23:683-91.
[Google Scholar]
|
| 32. |
Gladman DD. Psoriatic arthritis. Dermatol Ther 2004;17:350-63.
[Google Scholar]
|
| 33. |
Jones SM, Armas JB, Cohen MG, Lovell CR, Evison G, McHugh NJ. Psoriatic arthritis: Outcome of disease subsets and relationship of joint disease to nail and skin disease. Br J Rheumatol 1994;33:834-9.
[Google Scholar]
|
| 34. |
Elkayam O, Ophir J, Yaron M, Caspi D. Psoriatic arthritis: Interrelationships between skin and joint manifestations related to onset, course and distribution. Clin Rheumatol 2000;19:301-5.
[Google Scholar]
|
| 35. |
Reich K, Kruger K, Mossner R, Augustin M. Epidemiology and clinical pattern of psoriatic arthritis in Germany: A prospective interdisciplinary epidemiological study of 1511 patients with plaque-type psoriasis. Br J Dermatol 2009;160:1040-7.
[Google Scholar]
|
| 36. |
Gladman DD, Anhorn KA, Schachter RK, Mervart H. HLA antigens in psoriatic arthritis. J Rheumatol 1986;13:586-92.
[Google Scholar]
|
| 37. |
Scarpa R, Oriente P, Pucino A, Torella M, Vignone L, Riccio A, et al. Psoriatic arthritis in psoriatic patients. Br J Rheumatol 1984;23:246-50.
[Google Scholar]
|
| 38. |
McGonagle D, Tan AL, Benjamin M. The nail as a musculoskeletal appendage - implications for an improved understanding of the link between psoriasis and arthritis. Dermatology 2008;218:97-108.
[Google Scholar]
|
| 39. |
Helliwell PS, Marchesom A, Peters M, Barker M, Wright V. A re-evaluation of the osteoarticular manifestations of psoriasis. Br J Rheumatol 1991;130:339-45.
[Google Scholar]
|
| 40. |
Veale D, Rogers S, Fiztgerald O. Classification of clinical subsets in psoriatic arthritis. Br J Rheumatol 1994;33:133-8.
[Google Scholar]
|
| 41. |
Thumboo J, Tharn SN, Tay YK, Chee T, Mow B, Chia HP, et al. Patterns of psoriatic arthritis in Orientals. J Rheumatol 1997;24:1949-53.
[Google Scholar]
|
| 42. |
Salvarani C, Scocco GL, Macchioni P, Cremonesi T, Rossi F, Mantovani W, et al. Prevalence of psoriatic arthritis in Italian psoriatic patients. J Rheumatol 1995;22:1499-503.
[Google Scholar]
|
Fulltext Views
6,535
PDF downloads
2,557





