Translate this page into:
Kindler's syndrome with long thick cuticles and mottled hyperpigmentation
Correspondence Address:
Devraj Dogra
Department of Dermatology Venereology and Leprology, Government Medical College and Associated Hospitals, Jammu
India
| How to cite this article: Gupta V, Dogra D, Gupta N, Parveen S. Kindler's syndrome with long thick cuticles and mottled hyperpigmentation. Indian J Dermatol Venereol Leprol 2011;77:66-68 |
Sir,
Kindler′s syndrome is a rare genodermatosis characterized by congenital acral blistering, photosensitivity and later by the development of progressive diffuse poikiloderma and cutaneous atrophy. [1] The other associated findings include periodontal disease, ophthalmic and mucosal abnormalities, palmoplantar keratoderma, webbing of fingers and toes, and rarely, nail changes. [2] We report the case of a 4-year-old female child with characteristic features of photosensitivity, acral blistering, cutaneous atrophy and early poikilodermatous changes. In addition, our patient had long thick cuticles, which is rarely reported. [3]
A 4-year-old female child, born out of non-consanguineous marriage, presented with spontaneous, recurrent blistering over extensor aspect of forearms, lower legs and dorsum of hands and feet since early neonatal period. The blisters used to rupture within 4-5 days to produce erosions which healed with hypopigmentation and atrophy. The episode of blistering continued to occur after every 2 months with no seasonal variation. At about 1 year of age, parents noticed diffuse hyperpigmentation over face and mottled hyperpigmentation over the neck, trunk, buttocks and thighs. For last 1 year, her skin over dorsum of hands and feet became thin, wrinkled, scaly and roughened. Along with this, the child developed severe itching over face, more on sun exposure. There was no similar illness in the family.
General physical and systemic examination was normal with grade one malnutrition and normal mental development. Cutaneous examination revealed diffuse hyperpigmentation over face and helices of ear lobes with interspersed areas of hypopigmentation, telengiectasias and epidermal atrophy. In addition, similar poikilodermatous changes were present over neck, upper chest and upper back [Figure - 1]. Unusual multiple irregular, light brown macules of 2-5 mm size were present over trunk, buttocks and proximal limbs [Figure - 2]. Marked cutaneous atrophy along with multiple crusted erosions were present over dorsum of fingers and toes. Mild palmoplantar keratoderma along with webbing between 2 nd and 3 rd and 3 rd and 4 th toes of both feet was present. Nails were apparently normal except for the long and thick cuticles present in most of the fingers and toes which had covered almost one-third to half of the nail plate and had smooth surface and sharp non-fragile distal edge [Figure - 3]. Her eye, dental, oral and genital mucosal examinations were normal.
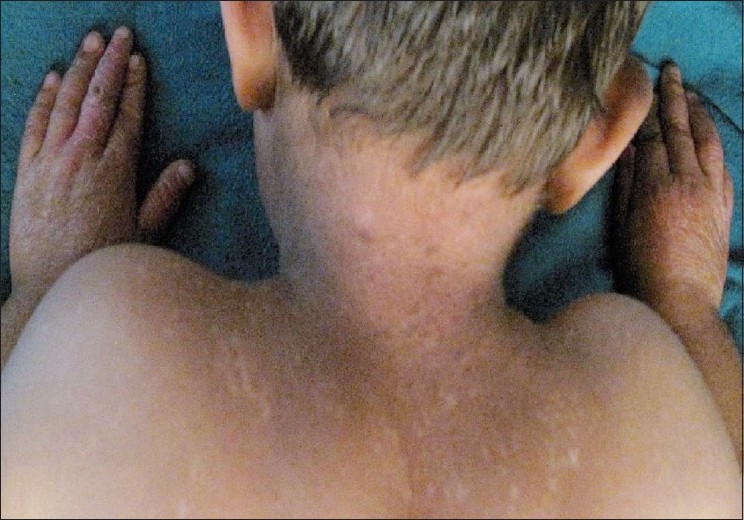 |
| Figure 1 :Early poikilodermatous changes on the upper back and neck |
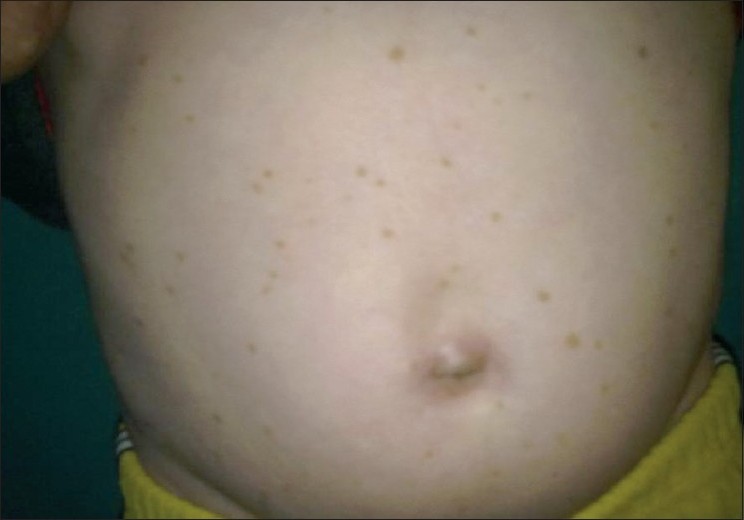 |
| Figure 2 :Mottled hyperpigmentation and discrete hyperpigmented macules on the abdomen |
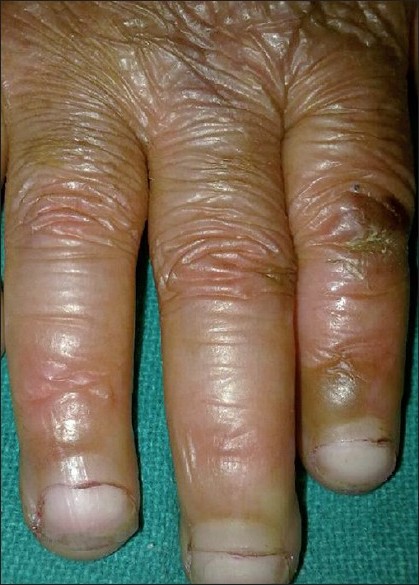 |
| Figure 3 :Long and thick cuticles covering up to half of the nail. Note cigarette paper like atrophy over dorsa of fingers |
Her complete hemogram, liver and renal function tests and urine analysis were within normal range. Qualitative tests for porphyrin in blood and urine were negative. The histopathologic examination from light brown macule over trunk showed mild hyperkeratosis and acanthosis of epidermis with increase in number of melanocytes at the basal layer. Immunofluorescence from uninvolved skin over inner aspect of upper arm was negative for IgM colloid bodies. Symptomatic treatment was given to the patient with an advice to avoid trauma and direct exposure to sunlight and to use calamine lotion liberally to slow down the progression of poikiloderma.
Kindler′s syndrome, first described by Theresa Kindler in 1954 in a 14-year-old girl, is an extremely rare genetic disorder with features of epidermolysis bullosa and poikiloderma congenitale. [1] Most patients with Kindler′s syndrome usually have a combination of four major features which include acral blistering in infancy and childhood, progressive poikiloderma, skin atrophy and abnormal photosensitivity. [2],[4] The common associated features include ophthalmic and mucosal changes, skin fragility, palmoplantar keratoderma, webbing of fingers and toes, and rarely, nail changes. In addition to the four major criteria, our patient presented with circumscribed hyperpigmented macules on trunk and long thick shiny cuticles of nails.
The genetic basis of Kindler′s syndrome involves a gene called KIND1, identified on chromosome 20p12.3 which encodes kindlin-1 protein, a component of focal contacts in keratinocytes expressed in the epidermis, particularly in the basal keratinocytes. Loss of this protein results in abnormal skin fragility with defects in actin-extracellular matrix linkage. [5] Both blistering and photosensitivity begin in infancy or early childhood and improve significantly with age, whereas poikiloderma appears gradually initially over sun exposed areas and becomes more prominent later in life to involve non-exposed areas also. [2],[4] Atrophic changes, cigarette paper like wrinkled appearance of the skin are most pronounced on the dorsa of the hands and feet. Sclerodermoid changes of the fingers and nails have also been reported. [2]
Dental abnormalities have been reported to occur commonly in affected patients. Ophthalmic abnormalities have also been described in some patients. [4] No such abnormalities were present in our patient. Mucosal involvement in the form of leukokeratosis of buccal mucosa, urethral, anal, and esophageal stenosis has been reported. [2],[4] Mucous membranes were normal in our patient.
Less common and variable features reported include palmoplantar hyperkeratosis and webbing of fingers and toes. This webbing has been attributed to the trauma of repeated blistering and scarring in infancy. [2]
Multiple scattered, mottled hyperpigmented macules distributed over trunk and proximal limbs were seen in our patient. Similar finding has also been reported by Has et al. [5] who considered it to be an early sign of poikilodermatous changes over the covered areas, which develop later.
Nail changes in Kindler′s syndrome, although rare, have been described. [3] In our patient, long and thick cuticles were seen in most of the nails. Similar finding was also noted by Nath et al.[3] They speculated whether this was an incidental finding or a feature of nail involvement in Kindler′s syndrome. Finding in our patient supports the latter view. Atrophy of the living layers of the skin and relative sparing of dead horny layer, which forms the cuticle of the nail, is thought to be responsible for this change in cuticles. [3]
| 1. |
Kindler T. Congenital poikiloderma with traumatic bulla formation and progressive cutaneous atrophy. Br J Dermatol 1954;66:104-11.
[Google Scholar]
|
| 2. |
Penagos H, Jaen M, Sancho MT, Saborio MR, Fallas VG, Siegel DH, et al. Kindler's syndrome in native Americans from Panama. Arch Dermatol 2004;140:939-44.
[Google Scholar]
|
| 3. |
Nath AK, Chougule A, Thappa DM. Long cuticle of the nail in Kindler's syndrome: Is it more than an incidental finding? Indian J Dermatol Venereol Leprol 2009;75:314-5.
[Google Scholar]
|
| 4. |
Nofal E, Assaf M, Elmosalamy K. Kindler syndrome: A study of five Egyptian cases with evaluation of severity. Int J Dermatol 2008;2:289-93.
[Google Scholar]
|
| 5. |
Has C, Tuderman LB. A novel nonsense mutation in Kindler's syndrome. J Invest Dermatol 2004;122:84-6.
[Google Scholar]
|
Fulltext Views
3,054
PDF downloads
1,921





